Clinic for Implant
&
Orthodontic Dentistry, procedures explained, offers, information,
Creating Perfect Dentures at Home with a Dentist Who Comes to You- By Dr Amir Mostofi DDS Dip MSc
Creating custom dentures at home with the expertise of a domiciliary dentist is an ideal solution, especially for patients facing unique challenges. Clinic for Implant & Orthodontic Dentistry prioritises patient-centred care, ensuring the utmost comfort and satisfaction throughout the process. Our journey begins with a comprehensive initial consultation, followed by extractions if necessary. Accurate impressions of your jaw are taken, even in cases of shrinking jawbones. We provide flexibility, allowing alterations during the wax trial denture stage at no extra cost. For those with cobalt chrome dentures, we handle the challenges seamlessly. We also offer domiciliary dental care for home-bound or bed-bound patients, ensuring safety and convenience. Our goal is to craft dentures that restore your smile and improve your quality of life.
Creating Perfect Dentures at Home with a Dentist Who Comes to You
Dentures made in the convenience of one's own home with the assistance of a domiciliary dentist are an excellent option for those who find traditional dental visits difficult. At Clinic for Implant & Orthodontic Dentistry, we specialise in providing denture services that are tailored to the specific requirements of our patients, including those with dementia and other mental disorders. In this exhaustive guide, we will walk you through the various phases of denture creation, from initial consultations to the final fitting, while emphasising the significance of a domiciliary dentist's experience in managing complex cases.
Step 1: Consultations at the outset
The initial consultation is a crucial first stage in the process of acquiring dentures. During this appointment, our domiciliary dentist conducts a comprehensive examination of your oral health and discusses the denture options that best meet your requirements. For a number of our patients, particularly those with dementia, collecting impressions can be difficult. Our experienced domiciliary dentists play a crucial role in the management of such cases. During this phase, we also ensure that all necessary documentation, including consent forms and cost discussions, is completed.
Step 2: Extraction, if Required
When oral health issues are identified during the initial consultation, tooth extraction may be required. To minimise patient distress, tooth extraction is performed with care and frequently in stages. This period, which typically lasts between one and three weeks, allows the mouth to recuperate and reduces swelling, making future dentures fit better.
Step 3: Taking Impressions
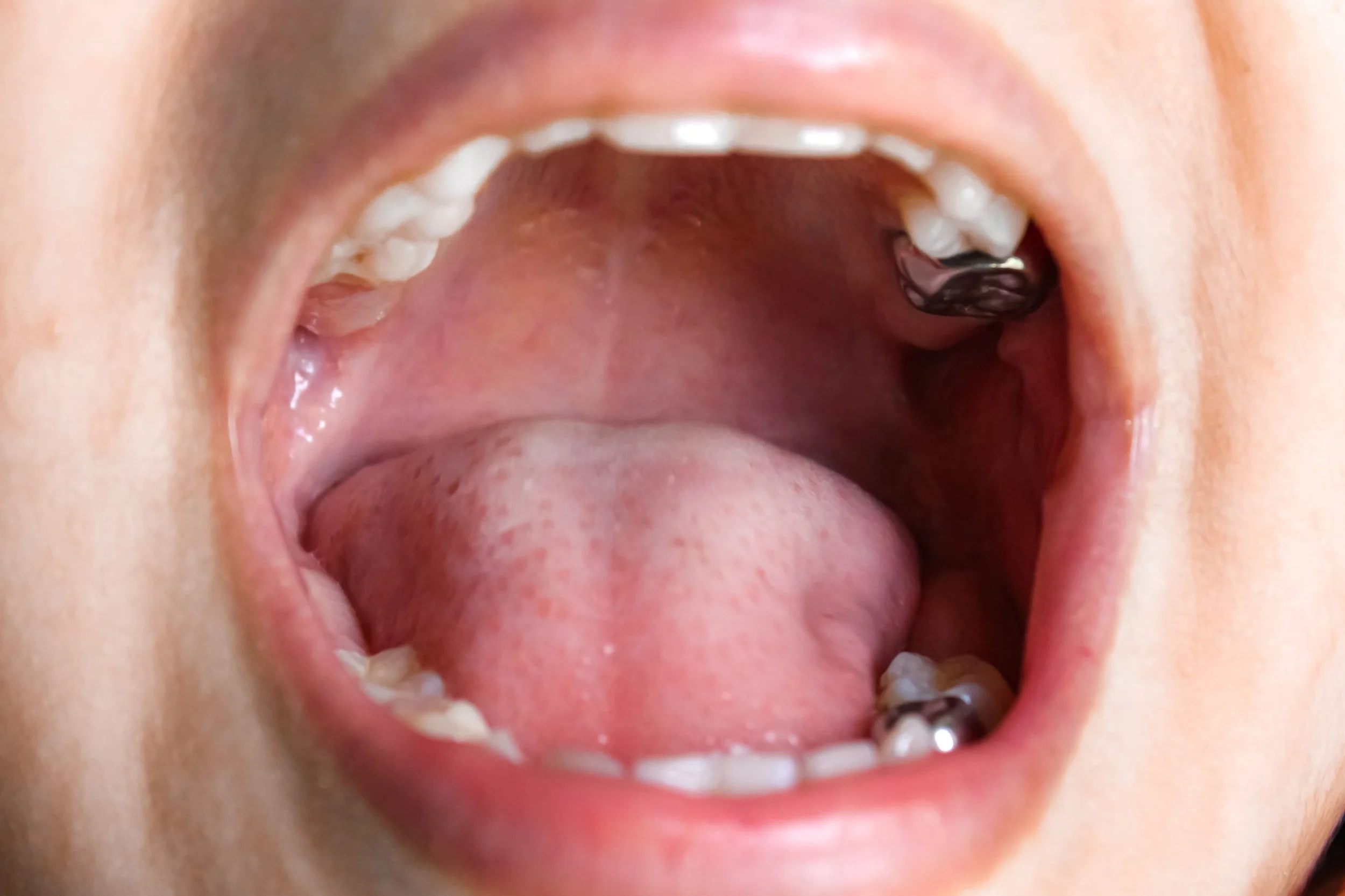
Taking accurate impressions of your upper and lower mandible is a crucial step in the fabrication of dentures that fit securely and comfortably. Numerous elderly individuals struggle with thinning jawbones, necessitating the use of specialised impression-taking techniques. Our domiciliary dentists are well-versed in adapting these techniques to individual requirements, thereby ensuring an accurate representation of your mandible and any remaining teeth.
Step 4: Registration of the Bite
At the stage of bite registration, the complex relationship between your upper and lower mandible is established. This procedure enables the dentist to record the precise relationship between your jaws. In addition, during this phase, the colour, shape, size, and quality of the denture teeth are meticulously determined, ensuring that your dentures appear and feel natural.
Step 5: Wax trial dentures
Seeing the wax trial dentures in your mouth is a crucial step in the process of creating dentures. This phase enables both you and the dental technician to evaluate whether the desired aesthetic has been achieved. At this juncture, any necessary modifications can be discussed and implemented. At Clinic for Implant & Orthodontic Dentistry, we prioritise your satisfaction, and alterations are made at no additional cost if necessary.
Step 6: Final Fitting and Adjustments
In the final stage, the completed dentures are adjusted. If significant changes were made during the wax trial denture stage, it may be necessary to repeat appointment 4. We recognise that the process of having dentures fitted can be intimidating, especially for first-timers or those who have had negative experiences in the past. Our dedication to ensuring that you comprehend the procedure and our emphasis on both form and function ensure that you leave with dentures that inspire confidence.
Visits and Problems with Cobalt Chrome Dentures
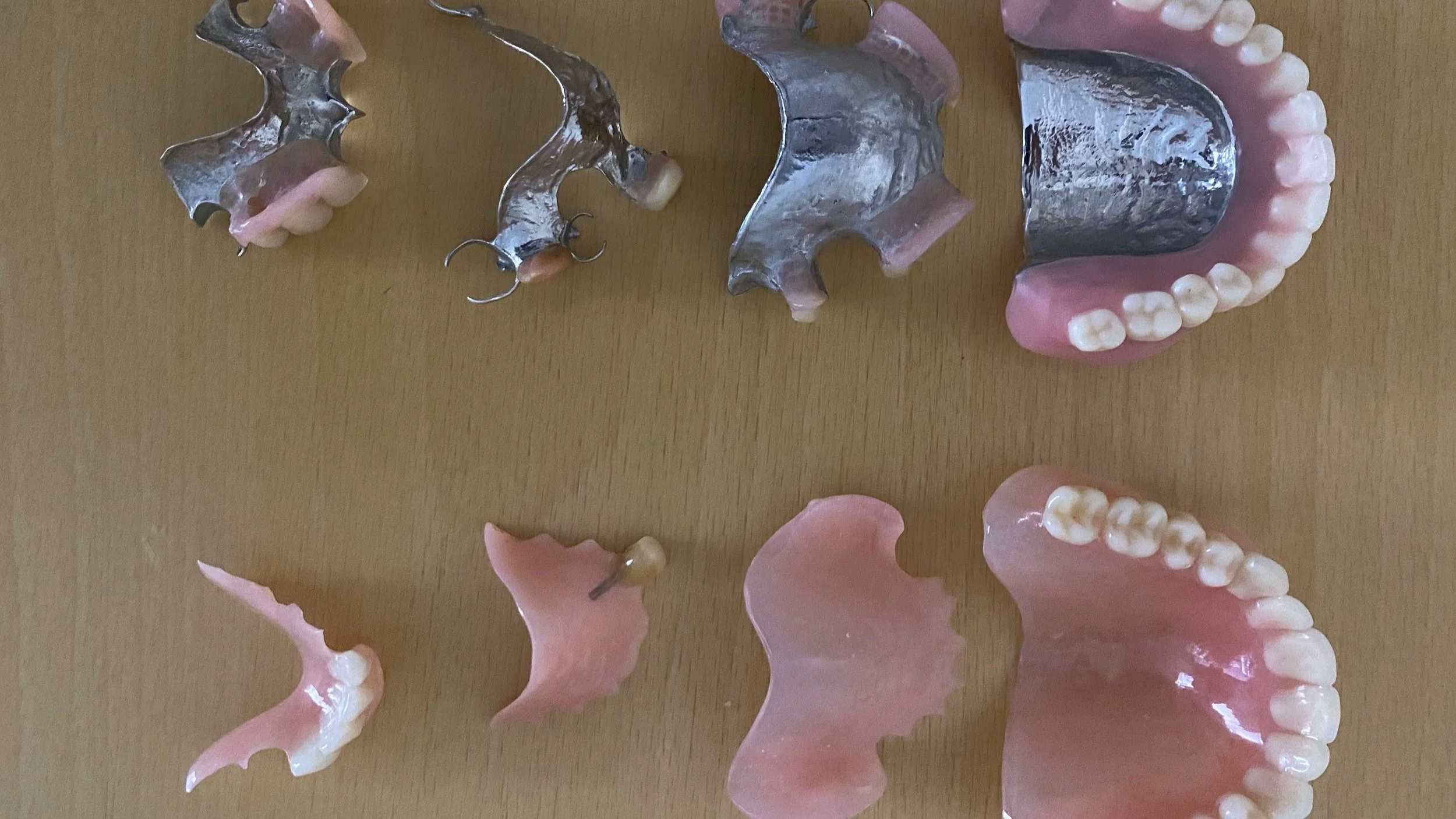
Generally, between four and seven visits are required to complete a denture, depending on the individual's requirements and complexity. However, cobalt chromium dentures, which contain a metal skeleton, typically require more visits due to the complexity of their fabrication and adjustment. Our skilled team at Clinic for Implant & Orthodontic Dentistry is well-equipped to handle such challenges, assuring the best possible outcome for your cobalt chrome dentures.
Domiciliary dental care for patients confined to their homes or beds
We recognise that not all patients have easy access to dental clinics. For this reason, we offer home visits, also known as domiciliary dental care, to those who are bedridden or confined to their homes. We make the process as convenient and comfortable as possible for patients who can recline in a wheelchair or regular chair with space around the dentist's workspace.
If a patient is completely bedridden and inclining the bed is not an option, we do have a solution. We use intraoral digital scanners as opposed to traditional impression materials, thereby eliminating the danger of material running down the patient's throat and ensuring a safe and efficient procedure.
The conclusion
A personalised and patient-centered approach to dental treatment is the fabrication of dentures in the patient's residence by a domiciliary dentist. At the Clinic for Implant & Orthodontic Dentistry, we strive to make this journey as pleasant and rewarding as possible, particularly for patients confronting unique obstacles. We have the knowledge and skill to create dentures that restore your smile and improve your quality of life. If you would like to schedule an initial consultation, please contact us at 01903-821822. We anticipate serving you and ensuring that your dental requirements are met with the utmost care and expertise.
Top 5 Sources of Dental Implant Pain When "There's Nothing Wrong with the Implant"- By Dr Amir Mostofi, DDs Dip MSc
Experiencing pain after a dental implant, even when everything looks fine? Explore the top 5 reasons behind post-implant discomfort and find solutions to ensure a comfortable journey towards a perfect smile.
If you've recently had a dental implant and are experiencing pain even though everything seems normal, you're not alone. This article aims to explain the top 5 reasons behind dental implant pain when there's no apparent issue with the implant itself, in a way that's easy for patients to understand.
1. Violations of the Inferior Alveolar Canal (IAC):
The IAC is a canal that houses the inferior alveolar nerve (IAN), which plays a crucial role in sensation for your lower jaw. Sometimes, the IAN takes a unique path, forming what's called an "anterior loop." Trauma to this area during implant placement can lead to sensory disturbances, bleeding, and pain. Recent research suggests that getting closer to the IAC may not be as risky as previously thought, as long as the nerve isn't directly affected.
2. Violations of Branches in the Mandibular Canal:
Traditionally, we've considered the IAC as a single canal to be avoided during implant surgery. However, it's now known that smaller branches can exist alongside the main canal, creating a network. If these branches are accidentally disturbed during surgery, it can result in pain. These branches are often missed because they aren't widely recognized, but they can show up on X-rays or CT scans.
3. Inadequate Keratinized Tissue:
Keratinized tissue is the protective, tough tissue that surrounds your implant crown. Some studies suggest that not having enough of this tissue (usually at least 2 mm wide) can lead to pain, especially when you touch or use the implant, like when brushing or eating. Fortunately, this issue can often be resolved by adding more tissue through a soft-tissue graft.
4. Poor Bone-to-Implant Contact:
Even if an implant looks fine on X-rays and CT scans, it's possible that the bone around it isn't providing a secure foundation. This can happen when fibrous tissue forms around the implant instead of sturdy bone. This may not be visible in regular exams, but patients can still feel pain when using their implant, especially when it's fitted with a crown. A resonance frequency analysis machine can help diagnose this issue by measuring the strength of the implant-bone connection.
5. Predisposing Risk Factors:
Sometimes, pain after implant surgery can be linked to factors that exist within your medical or genetic makeup. Conditions like fibromyalgia, temporomandibular disorders, and depression/anxiety can make you more prone to experiencing pain. This type of unexplained pain often falls under the category of "peripheral painful traumatic trigeminal neuropathy" (PPTTN).
In summary, if you're feeling pain after a dental implant, even when everything looks fine, it's important to consider these factors before assuming it's psychosomatic. There are various reasons behind implant-related pain, and a thorough evaluation is essential to pinpoint the cause accurately. Your dental professional can help you identify and address the issue, ensuring your dental implant journey is as comfortable as possible.
Dental Care for Elderly Patients with Alzheimer's and Dementia in Nursing Homes: The Importance of Experience and Adaptation- By Dr Amir Mostofi, DDS Dip MSc
Caring for elderly patients with Alzheimer's and dementia in nursing homes presents unique challenges, especially when it comes to their dental care. In this article, we explore the importance of dentists with experience treating this vulnerable patient group and their ability to adapt their diagnostic and treatment planning approaches. These patients face multiple dental issues, including tooth decay, gum disease, dry mouth, and difficulties with chewing and swallowing. Dentists familiar with their unique needs possess specialised knowledge, communicate effectively despite the patients' limited ability to express discomfort, and provide gentle care that considers their fragility.
Caregiving for geriatric patients with Alzheimer's and dementia in nursing homes presents unique challenges, particularly in the area of dental care. Due to their medical conditions, these individuals frequently experience a variety of dental issues, including tooth decay, periodontal disease, dry mouth, and difficulty chewing and swallowing. This article will explore the significance of dentists who have experience working with this vulnerable patient population and how they navigate the complexities of diagnosis and treatment planning while taking into account their fragility and inability to communicate pain.
Understanding the Dental Concerns of Elderly Alzheimer's and Dementia Patients:
Patients with Alzheimer's disease and dementia are susceptible to a variety of dental issues, including:
Dental Decay: Numerous factors, including poor oral hygiene, consumption of sugary foods, and medication adverse effects, contribute to tooth decay. Additionally, Alzheimer's and dementia patients may have difficulty maintaining appropriate oral hygiene.
Poor oral hygiene can result in gum disease, which can result in discomfort, oozing gums, and even tooth loss. The limited motor skills and cognitive decline of these patients may make it difficult for them to perform adequate oral hygiene.
Reduced saliva production is a prevalent problem among Alzheimer's and dementia patients. As saliva serves to neutralise acids and protect teeth, dry mouth can increase the risk of tooth decay and gum disease.
Cognitive decline and motor skill impairments can impair a patient's ability to correctly chew and swallow. This can lead to malnutrition and pneumonia from aspiration.
Dentists with experience in treating elderly patients with Alzheimer's and dementia play an essential role in providing effective and compassionate dental care. Here's why their experience is significant:
a. Specialised Knowledge: These dentists have an in-depth comprehension of the unique dental issues confronted by Alzheimer's and dementia patients. They are aware of the potential oral health complications associated with cognitive decline and are able to anticipate and proactively address them.
b. Communication and Adaptation: Patients with Alzheimer's and dementia may have difficulty expressing pain or distress; therefore, dentists must be adept at interpreting nonverbal cues and behaviour. Dentists with experience are able to modify their diagnostic methods to guarantee precise evaluations and develop treatment plans accordingly.
c. Fragility and Patient Comfort: The geriatric patients with Alzheimer's and dementia require gentle and compassionate dental care due to their fragility. Dentists with extensive experience are well-versed in handling these patients with care, employing techniques that minimise anxiety and pain throughout the treatment.
d. Collaborative Approach: Dentists with experience in treating elderly patients with cognitive decline frequently collaborate with nursing home personnel and carers. This collaboration assures continuity of care, the exchange of vital information, and the development of individualised treatment plans tailored to the specific needs of the patient.
Importance of Diagnosis and Treatment Planning: Diagnosis and treatment planning for elderly patients with Alzheimer's disease and dementia must take into account their specific circumstances. Dentists must:
a. Conduct a Comprehensive Evaluation: Comprehensive dental examinations and evaluations are essential for identifying existing oral health issues and developing the most effective treatment plans. This evaluation should include a review of the patient's medical history, an assessment of their current dental health, and an evaluation of their oral hygiene practises.
b: Individualised Treatment: Each patient's treatment plan should be tailored to his or her particular requirements and limitations. Dentists must consider cognitive abilities, motor skills, and any medical conditions that could affect the quality of dental care provided.
c. Conservative Approaches: Given the fragility and potential distress of these patients, dentists may, whenever possible, opt for conservative treatment approaches. This may involve prioritising pain management, addressing essential issues first, and implementing preventive measures to ensure long-term oral health.
Dental care for Alzheimer's and dementia patients residing in nursing homes requires specialised knowledge, flexibility, and a patient-centered approach. Dentists with experience treating this population have the knowledge and skills necessary to provide comprehensive care while ensuring their patients' comfort and well-being. By recognising the significance of their role and adopting appropriate diagnostic and treatment planning strategies, dental professionals can substantially contribute to enhancing the oral health and overall quality of life of Alzheimer's and dementia patients.
A comprehensive patient guide for dental implants
In modern dentistry, dental implants have become the treatment of option for missing teeth. A dental implant is an artificial tooth root that is typically composed of titanium. When applied with skill, they provide a highly reliable treatment. The primary objective of implant placement is to obtain immediate, intimate contact with the surrounding bone. Over time, additional bone growth on the implant surface improves the implant's stability.
All There Is to Know About Dental Implants : A patient guide
In modern dentistry, dental implants have become the treatment of option for missing teeth.
What exactly is an implant?
A dental implant is an artificial tooth root that is typically composed of titanium. When applied with skill, they provide a highly reliable treatment. The primary objective of implant placement is to obtain immediate, intimate contact with the surrounding bone. Over time, additional bone growth on the implant surface improves the implant's stability.
In order to support replacement teeth, dental implants typically feature an internal screw thread or post space that permits the attachment of a variety of components. Once in place, these components provide long-lasting support for crowns, bridges, or removable dentures.
Who can receive dental implants?
Dental implants are appropriate for the majority of healthy adults. They can only be used once the jawbone has ceased growing, so they are typically not used on children. Habits such as excessive drinking or smoking can increase the number of complications associated with initial healing and may be detrimental to the gum and bone surrounding each implant in the long term. Smoking should be reduced or best still given up altogether. However, each case is unique, and if you have any medical issues, you should consult with one of our implant specialists prior to beginning treatment; in only a few instances do health issues completely preclude the use of dental implants.
Dental implants are appropriate for the majority of healthy adults.
How will you determine if you are a candidate for implants?
During your initial consultation, Dr. Mostofi will determine whether implant treatment is feasible. He will discuss your options and conduct an examination of your mouth and remaining teeth to determine the nature and extent of any existing dental issues. Typically, x-rays will be obtained, and dental models will be fabricated so that they can be examined after your appointment. These x-rays and models will be used to determine the optimal position for an implant, the number of implants required to fill the gap, and the available bone grade and volume.
Establishing excellent oral hygiene is a crucial step in any treatment plan. At this initial consultation, you will be informed of which problems are essential and what treatment is necessary to stabilise any gum or tooth issues.
Should you have a full mouth examination?
When you inquire about dental implants for the first time, it is frequently in response to ongoing dental issues or the recent loss of teeth. Before implant treatment, it will often be necessary to understand and treat the underlying cause of these issues.
If you have poor breath, loose teeth, or excessive bleeding, especially when your teeth are professionally cleaned, you may have gum disease.Gum disease (periodontal disease) is a leading cause of bone loss, making dental implant treatment more difficult, but not impossible.
How lengthy is the treatment?
For routine cases, the duration between implant placement and the placement of the first tooth/teeth can range from three to six months. The availability of higher-quality bone can be used to reduce treatment time, whereas inferior bone requires more time and care, which can extend treatment times beyond six months.
What should you understand before beginning treatment?
You will receive a summary of your discussion regarding treatment planning, emphasising your current dental condition and any alternatives to dental implants. This summary also provides an overview of the anticipated treatment stages and provides an estimate of the expected duration, number of implants, and cost. There may be additional issues unique to your case, and they will be addressed accordingly.
How long do implants typically last?
Once the implants and surrounding soft tissues are deemed to be healthy and the new teeth are deemed to be comfortable and properly aligned, the quality of your oral hygiene and willingness to attend regular maintenance reviews will have the greatest impact on their longevity.
Similar to neglected natural teeth, implants will develop a layer of hard and porous deposits (calculus and plaque) if they are not properly cared for. These deposits, if left untreated, can cause gingival infection, bleeding, soreness, and general discomfort. Implants could be said to have the same longevity as natural teeth. Implants that are well-maintained and placed in sufficient bone can potentially last a lifetime if cared for properly. However, just as you would anticipate traditional crowns, bridges, and fillings to require occasional restorations or replacements, implant-supported teeth may also require similar maintenance over time.
How many teeth can dental implants support?
Dental implants can be used to replace a single tooth or an entire arch of teeth. Dental implants can support all prevalent forms of tooth replacement, such as bridges and dentures. If you are missing a single natural tooth, one implant will typically suffice to provide a replacement. However, larger spaces created by two, three, or more missing teeth may not require one implant per tooth; the precise number of implants will depend on the grade and quantity of bone at each potential implant site.
Patients with a propensity of clenching or grinding their teeth (bruxism) may be at risk of implant overload. Bruxism occurs during sleep for most individuals, so they are typically unaware of it. The most common clinical indications of bruxism are excessively worn or flattened teeth, chipped enamel edges, and/or the frequent breakage of filling fragments. During treatment planning, the effects of bruxism must be considered, and they can be compensated for by placing additional implants, selecting appropriate restorative materials, and providing a nighttime bite guard to secure the new teeth. This will be covered in your initial consultation and treatment plan.
Implant retained prostheses
What are implant retained dentures?
Using dental implants to anchor removable prostheses (dentures) is a significantly more effective method than using adhesives, glue, or powders. With only two implants or four mini implants in each jaw, dentures can be clipped into position and held securely, but are simple to remove for cleaning and sleeping. Implants also provide a number of aesthetic advantages, including the preservation of bone in the jaw and the maintenance of facial structure, as well as the restoration of lost lip support to reduce wrinkles around the mouth. Approximately 2 hours procedure are devoted to actual surgery. It is a quick and economical alternative to a complete arch of dental implants.
What alternative treatments are available?
Implant-retained dentures are a significant improvement over traditional removable dentures, which are inconvenient, sometimes uncomfortable, and restrict your diet. Full arch dental implants are an even better alternative to removable dentures; we are one of the few practises in West Sussex with the expertise to conduct this procedure. It's a life-altering, permanent solution.
Is it essential to replace an entire set of lacking teeth?
Multiple tooth loss can have a profound effect on one's quality of life. In addition to having a significant influence on your ability to speak and eat, it can also alter your appearance. Without teeth to support the lips and cheekbones, wrinkles develop more quickly and the cheeks become hollow. Many individuals with this type of tooth loss believe they appear older than they are, which can be detrimental to their self-esteem.
A summary of the implant procedure
Typically, implant treatment consists of several phases that occur over a period of three to nine months. Although there are numerous implant treatment methods, a typical procedure typically involves the following:
Assessment and planning for treatment:
At the initial consultation, after a thorough discussion of all potential alternatives, we will determine whether implant treatment is feasible. If necessary, x-rays will be obtained and models of the teeth will be created. Then, a written treatment plan detailing the treatment sequence and associated costs will be created.
Implant placement:
Implant implantation is a relatively straightforward minor surgical procedure that can be performed in a dental office under sterile conditions. The procedure is performed under local anaesthesia and, if necessary, sedation. If, during evaluation, it is determined that the underlying bone is deficient, there are several options for bone regeneration. Depending on the needs, bone regeneration is typically performed at the same time as implant placement.
Healing or Transition period:
It can take between six weeks and six months for implants to integrate with a patient's bone. During this period of integration, temporary dentures or bridgework may be worn as needed. In certain instances, temporary teeth can be affixed to the implants in a procedure known as "immediate loading" while the implants integrate.
The Recuperative stage:
Once implants are incorporated, they can be restored with a variety of new teeth (definitive restorations) including a single crown, small or large bridge, or removable overdenture. We collaborate closely with a laboratory that creates these permanent restorations.
Maintenance:
Following conclusion of implant treatment, the patient must clean the new teeth (restorations) according to the instructions. A dental hygienist may also provide guidance on the care and upkeep of restorations and natural teeth. Regular visits to the dentist are required so that the health of the soft tissues, bone levels, and restoration can be evaluated.
How can you determine if you have sufficient bone for dental implants? Normal dental x-rays display a great deal of detail, but only in two dimensions. From these views, it is typically possible to determine the height of available bone for implant placement; however, sometimes more advanced imaging techniques are required to determine the equally crucial bone breadth.
Dental CBCT Scans – there are now a number of sophisticated x-ray techniques that enable a three-dimensional examination of the jawbone. CBCT (cone beam computed tomography) scans are the most precise and widely available. Images obtained by CBCT scanning will typically display all of the necessary bone information, including quantity and quality, but most importantly, the presence of structures that must be avoided.
What may result in bone loss?
When a tooth is lost or extracted, a significant portion of the bone that once encompassed the remaining root may be lost. This loss is referred to as "bone resorption" and can be especially rapid during the first few months. Despite the fact that the rate and quantity of bone resorption are highly variable between individuals, it will always occur to some degree unless special precautions are taken to mitigate its effects.
Many patients report that their dentures gradually become looser and no longer fit as well as they once did. Initially, the observed worsening of denture fit was a result of the increased rate of bone loss following tooth extractions. It is the direct effect of gnawing forces that causes the gradual deterioration of supporting bone over time. Therefore, the longer prostheses are worn, the less available bone there is for dental implants.
What anatomical structures must be avoided during dental implant placement?
As long as the implants remain within the bone that once supported your natural teeth, there are no significant risk areas in the upper mandible. If you are missing upper back teeth, you can be shown the contour and location of the area above the roots (maxillary sinuses). Since the maxillary sinuses are visible on the majority of x-rays, they are generally avoided.
The 'inferior dental nerve' is the most vital anatomical structure to avoid in the lower mandible. This nerve begins behind the wisdom teeth, travels under the back teeth (molars), and emerges on the epidermis of the face where the middle teeth (premolars) are or were. This is the reason why a normal dental anaesthetic numbs the lip even when the needle is inserted in the very back of the mouth. If this nerve is irritated or damaged during dental implant implantation, it can result in temporary or permanent numbness or altered sensation. This is an uncommon but significant complication.CBCT scans are typically the most accurate method for pinpointing the location of this nerve, allowing implants to be implanted with confidence. CBCT scans are more expensive than standard dental x-rays, but the information they provide is often invaluable for complex treatment planning and determining the location of vital anatomical structures. If a tooth is inadvertently damaged by the implantation of a nearby implant, any resulting issues can typically be treated with root canal therapy, in which the tooth's nerve is removed.
Can dental implants preserve bone?
This is one of the most essential characteristics of dental implants. Once in place and supporting teeth, daily functional forces (eating, smiling, and speaking) stimulate the adjacent bone, causing it to become denser and stronger. As with all things, there are limitations to the amount of force an implant can exert. We will discuss this in greater depth as it pertains to your specific situation.
Can replacement teeth be worn while undergoing implant treatment?
If the teeth being replaced by dental implants are in a highly visible area of the mouth, it is probable that you will need to have some teeth present during the procedure. This can be accomplished in a variety of ways, ranging from simple plastic dentures to removable bridges. If replacement teeth are used during treatment phases, it is vital that they do not exert uncontrolled pressure on the implants. You should anticipate a number of visits for minor adjustments to any temporary teeth after the implants are inserted and before they are activated. They might not be as visually appealing as your final restoration.
Are dental implants compatible with natural teeth?
Dental implants are routinely inserted adjacent to natural teeth, and this procedure is generally very safe. The only exception to this rule would be if the natural root was extremely curved or inclined in the proposed implant path. This could cause the implant to damage the root, but this is typically avoidable through meticulous pre-operative planning.
Are the replacement molars fused together?
When numerous implants are inserted, they are typically connected in the same manner as a bridge supported by natural teeth. When teeth supported by implants are joined together, they are mechanically sturdier than the sum of their parts.
If sufficient implants are available, it is frequently simpler and just as effective to construct several smaller bridge sections, each supporting a few teeth. The overall effect in the mouth is identical, and if you ever need to repair one of the minor sections, this can be accomplished much more easily. Again, the quality of the bone, as well as the number and placement of the implants, will determine which option is most suitable for you.
Is it unpleasant when implants are inserted?
The majority of patients will be familiar with the anaesthetics used in routine dentistry and will be aware of their efficacy. The same anaesthesia is used to insert implants. Depending on the complexity of your case, the procedure could last anywhere from 2 hours for a single implant to several hours for complex bone augmentation and the implantation of multiple implants. Expect some minor swelling and occasional discoloration after surgery. For the majority of patients, fundamental over-the-counter pain relievers will suffice for several days. If you continue to experience discomfort, contact your healthcare provider, who can prescribe a stronger medication.
Generally, healing is uncomplicated, and sutures are removed within ten to fourteen days. During the initial few days, you should disclose any unanticipated pain or swelling so that it can be evaluated. Always seek advice when in doubt, as early detection of a problem often leads to a simplified solution. You may also be prescribed antibiotics and asked to perform some basic procedures, such as rinsing your mouth with salt water or an antiseptic mouth rinse. It is essential that you follow these directions.
If the implant surgery will take a long time, is sedation an option?
Although it is relatively simple to provide effective pain management during surgery, the majority of patients will be apprehensive. There is no need to suffer in silence, as there are numerous highly effective ways to attain a state of relaxation.
Conscious sedation – For more complex procedures, it may be recommended that you have a more regulated method of relaxation and comfort during the surgical phases. This is known as 'conscious sedation' and is distinct from a anaesthetic because you are awake enough to respond to simple instructions that may be helpful to the surgeon; however, you will recall almost nothing of the treatment phase. It is especially advantageous for procedures lasting more than an hour that do not require hospitalisation; this is likely the case for the majority of dental implant treatments. For routine "conscious sedation," a sedative is administered via an arm or hand vein for the duration of the procedure. An anesthesiologist continuously monitors your pulse rate and oxygen levels during this extremely safe procedure. A standard dental local anaesthetic is injected around the proposed implant sites under conscious anaesthesia. By the time the dental anaesthetic is administered, the anaesthetic has already taken effect, so most patients do not recall this phase. For procedures requiring oral or conscious anaesthetic, you may be asked to refrain from eating or drinking for at least four hours prior to surgery, and you will be required to make arrangements for an adult to drive you home. Additionally, you will be instructed not to operate any apparatus for at least 24 to 36 hours.
What can be done if there are insufficient bones?
Up to this point, we have covered the fundamentals of routine implant placement. This has included the initial examination and diagnosis, special x-rays such as CBCT scans, anaesthesia during surgery, and what to expect following the placement of implants. However, for some individuals, bone loss following tooth extraction or loss prevents the placement of an implant. There are actions that can be taken if this occurs:
It is possible to increase the height of the available bone in the upper jaw above the back molars by creating new bone in the sinus. This process is known as "sinus augmentation." Without the widespread success of this technique, numerous patients would be unable to receive dental implants in a region of the mouth where tooth loss is so prevalent.
There are numerous methods for adding bone, but one of the simplest is to remove a piece of bone from another location and attach it as an "onlay graft" to a deficient area. The new piece of bone will gradually fuse with the underlying bone, and an implant can be implanted in a more favourable position once it has healed and matured.
Where can additional bone be obtained?
Bone can be harvested from a variety of locations, but most commonly from the back of the lower mandible or the chin. Occasionally, it is extracted from the hip or tibia. When using your own bone to create new bone in another area of the mandible, you will experience discomfort at both the donor site and the surgical site. As your own bone is typically regarded as the 'gold standard,' many people feel that the additional discomfort is well worth it.
Alternatives to your own bone for augmentation There are other sources of bone, such as bovine (derived from cows), porcine (derived from pigs), and synthetic materials that have been specially processed to make them acceptable for use in humans, for those who prefer an easier but slightly slower solution. All of these materials, including your own bone, are merely scaffolds into which new bone will grow in a few months in preparation for dental implant placement.
It can take anywhere from three to twelve months for new bone to be suitable for dental implants. Do not rush to advance to the next stage. A larger quantity of bone will take longer to mature than a smaller quantity. Each surgeon will have a preferred technique for producing new bone. Many of them will additionally employ a technique known as "guided tissue regeneration." By placing a barrier material between slow-moving bone cells and the fast-moving cells of the soft tissues lining the mouth, this technique allows slower-moving bone cells time to occupy a space. This is a "resorbable barrier" that will dissolve spontaneously after a few months of performing its function.
Does bone augmentation impact treatment duration?
If you require bone augmentation, it may lengthen the duration of your treatment; however, when performed successfully, it will significantly enhance the outcome of the implant(s) placed. When used in the front of the mouth, it can also enable the construction of much more aesthetically pleasing results.
Regardless of the method selected to increase bone density, the time, effort, and expense are generally worthwhile.
How do you care for your implants?
To increase the longevity of your implants, it is imperative that you maintain excellent oral hygiene. Cleaning your implants is straightforward. For the majority of implant-supported teeth, you will be able to brush and floss around each supporting implant just as you would around natural teeth and tooth-supported bridges. Maintaining excellent oral hygiene may require special floss, interdental toothbrushes, and other cleaning aids in some areas.
If you wish to maintain optimal implant health, it is reasonable to anticipate that some daily maintenance procedures will be more complex than those performed around your natural teeth, and that you will need to devote more time than in the past.
During the first few months following implant placement, your dentist may request that you visit them more frequently; however, once they are satisfied that your treatment is proceeding according to plan, your ongoing dental care will be comparable to that of a patient with natural teeth.
What options exist if an implant fails?
The average success rate for dental implants is approximately 90%; you should discuss how the loss of an implant could affect your treatment plan. A dental implant can fail for a variety of reasons, including smoking, poor oral hygiene, and systemic disease. In these particular high-risk groups, one would anticipate a much higher failure rate. If an implant does not integrate well with the surrounding bone, it will ultimately lose its ability to support replacement teeth and become loose. Commonly, a failing implant does not cause discomfort, and if there are sufficient residual implants, it may not be necessary to replace it.
It is essential to discuss the potential complications that may arise.
Various implant procedures
One-stage implant – The implant is inserted into a fresh, healing, or healed extraction site where the original tooth was extracted, and is immediately visible above the gum. This technique has the advantage of not requiring a second surgical stage to expose the implant. Typically, the implant will not be able to sustain a tooth for several weeks or months.
This is the first stage of a two-stage implant, in which the implant is inserted into a fresh, healing, or healed extraction site and then concealed by a layer of gum tissue. At the second stage, weeks or months later, the implant is uncovered and components are added, bringing it to the surface of the gum so that a new tooth can be attached.
Same-day implants - necessitate meticulous planning prior to the actual day of surgery. A few hours after the placement of multiple implants, a full arch of temporary or permanent teeth can be affixed. If temporary dentures are used, they are typically replaced with a permanent bridge after a sufficient period of healing. Not all patients are appropriate candidates for this method of treatment.
In this procedure, a tooth is extracted and an implant is placed promptly into the extraction site. Depending on the local bone and soft tissue conditions, implant surgery may be performed in one or two stages. Not all patients are candidates for this treatment.
Immediate implant placement and early loading – This is dissimilar to immediate implant placement. It is essentially a one-step procedure in which the implant is inserted into a fresh, healing, or healed extraction site and a replacement tooth is attached at the same appointment. This first tooth will typically be kept out of direct contact with opposing teeth for more than three months, following which it will be restored. This procedure is more prevalent in areas of the mouth where aesthetics play an essential role. Again, this approach is not suitable for all patients.
Frequently asked questions:
Will I be able to consume my favourite foods afterwards?
Patients should be able to consume a normal, nutritious diet with little to no difficulty upon completion.
What are the costs associated with implant treatments?
The price can vary based on the required level and extent of treatment. A written treatment plan, therefore, explains and confirms the total cost.
How much time will it take?
Implant treatment typically requires multiple appointments over the course of several months. In certain instances, implant procedures can be completed much more quickly.
How long will an implant last?
Regular dental hygiene and regular check-ups should ensure that implants last for many years after treatment is complete.
Am I too elderly to receive implants?
There is no upper age limit for patients undergoing implant treatment, so long as they remain in reasonable health.
Is the procedure painful?
Patients are frequently astonished by the lack of pain they experience during and after implant procedures.
Glossary:
-Abutment
The abutment is the component that connects the implant to the permanent tooth restoration.
-Barrier membrane
A membrane that is draped over a bone defect or bone implant to prevent the infiltration of soft tissue, which could compromise the healing process.
-Bone augmentation
This is the insertion of natural or synthetic bone material in a deficient area of natural bone. This procedure may be performed concurrently with implant implantation, or as a separate procedure prior to implant placement.
-Bone resorption
Resorption of bone is the loss of bone height and/or width in the upper or lower mandible. This process continues throughout life, but is accelerated in areas where teeth have been lost.
-Bridge
A bridge is a method for replacing one or more missing teeth with artificial teeth that are bonded to adjacent natural teeth or dental implants. Bridges may be glued in position (adhesive bridges) or supported by crown preparations (conventional bridges) and constructed from a number of different materials.
-Bruxism
The act of clenching or grinding one's teeth when not chewing.
-Calculus
Sometimes referred to as tartar, tartar is a hard deposit that forms on teeth. Calculus is the result of the calcification of debris around the teeth, and it can be avoided by practising meticulous oral hygiene. Once calculus has formed, it is difficult to eradicate, and requires the services of a dental therapist or hygienist in most cases.
-Absolute arch
A complete arch refers to the teeth of the upper or lower mandible in their entirety.
-Consultation
A dental consultation to evaluate potential treatment options. Appointments may include an examination, x-rays, and photographs, as well as a frank discussion and explanation, if necessary.
-Crown
Crowns can be manufactured from a variety of materials, including porcelain, porcelain fused to metal, and gold. The majority of crowns that are not visible in the mouth are white in pigmentation.
-CBCT scan
Cone Beam Computed Tomography is a sophisticated x-ray technique that generates three-dimensional images of the mandible. Due to their three-dimensional nature, these images can only be observed on a computer screen.
-Definitive or final restoration
"Final restoration” refers to the ultimate implant-supported crown, bridge, or denture fabricated during the treatment process. The restoration will require routine maintenance and may require replacement.
-The administration of dental anaesthetics
Anaesthesia (Greek: ) means without sensation, which includes pain. The majority of dental anaesthetics are administered via injection into the affected area. Rarely, procedures may be performed while you are unconscious; this is known as a general anaesthetic.
-Dental implant
An implant is an artificial "tooth root." The majority of implants are composed of metal, with titanium or titanium alloys being the most prevalent. Implants are surgically inserted into the jawbone in order to support crowns and bridges or stabilise dentures.
-Dentures
Dentures are removable, custom-made replacement teeth. Typically, they are composed of acrylic or acrylic and cobalt chromium.
-Extraction
The extraction of teeth is the removal of teeth.
-Extraction position
The space left after tooth extraction.
Effective implantation
A functioning implant is one or more implants that are capable of supporting a dental restoration, such as a crown, bridge, or denture, and biting.
-Therapeutic tissue regeneration
A procedure that promotes the regeneration of soft tissue (gums) and may be used to improve the aesthetics around teeth or crowns.
-Gum disease
Soft tissue disease surrounding teeth. Gingivitis is the common name for gingival inflammation; it is a response to the deposition of plaque and, in most cases, can be treated with rigorous oral hygiene.
-Periodontal disease
Gingivitis can develop into periodontitis, a more severe form of gum disease, if left untreated. Periodontitis causes bone loss and can threaten the survival of a tooth or teeth.
-Immediate loading
Providing a temporary crown or bridge concurrently with implant implantation. Not all patients are appropriate candidates for this treatment.
-Inferior dental nerve
This nerve, sometimes known as the inferior alveolar nerve, travels through a bony canal in the lower jaw and provides sensation to the lower teeth, before emerging from bone as the mental nerve, which provides sensation to the lower lip.
**-Combination toothbrushes**
A small interdental brush with typically a single tuft of filaments. This can be used as an alternative to dental floss for cleansing between teeth and around implants.
**-Maximum sinus**
A hollow, air-filled space located just above the upper premolars. This varies in size from person to person and grows throughout one's lifetime.
**-Molars**
The upper and lower third molars on both sides of the mandible.
**-Onlay anastomosis**
When bone is taken from another area of the body, such as the hip (rarely), jaw, or behind the molars, and grafted to a deficient area.
**-Osseointegration**
Osseointegration is the bonding or fusion of an implant and bone, which typically takes several weeks to months.
**-Plaque**
Plaque is a soft, sticky, colourless film of bacteria that forms continuously on teeth and gums and can harden into calculus if not removed daily by practising good oral hygiene (brushing, flossing, etc.).
**-Premolars**
The two teeth located on both sides of the mandible in front of the molars.
**-Reline procedure**
During a relining procedure, a soft or firm material is used to correct the fitting surface of a denture following an extraction or surgery.
**-Removable overdenture**
A removable denture that is supported by implants but can be removed by the patient for cleansing.
**-Restorations**
The restoration may consist of a filling, a crown, a bridge, or a denture. It restores the tooth or teeth to full functionality.
**-Rejuvenating phase or appointment**
This phase follows the surgical phase of the treatment plan, typically a few weeks to a few months after a sufficient degree of recuperation. In the majority of instances, this will involve obtaining impressions so that the technician(s) can fabricate the definitive restoration.
**-Sinus augmentation**
A surgical procedure in which bone regenerative material is inserted into the sinus to stimulate the formation of new bone in order to enhance the available bone height for implant placement.
**-Sterile conditions**
In this context, sterility refers to the absence of bacterial contamination. We can never achieve absolute sterility, but we must always strive to achieve as near as possible to a sterile working environment. This includes the use of autoclaves to sterilise all nondisposable instruments as well as drapes and robes to isolate working surfaces and personnel.
**-Titanium**
This biocompatible metal is used to manufacture implants. Titanium has been utilised for decades in medical procedures, including hip replacements.
**-Treatment scheme**
A report outlining the patient's dental implant procedure, including the proposed treatment timeline and expenditures. The purpose of this guide is to provide an overview of standard dental implant treatment. Each individual's treatment plan for dental implants will be customised by Clinic for Implant & Orthodontic Dentistry in terms of cost, duration, and method of care delivery.
A Clinic for Root Canal Treatment Near You
The prospect of a first-time root canal can be daunting, but it offers a relatively quick and virtually painless solution when standard fillings can't save a tooth. Severe tooth pain, sensitivity, discoloration, and other symptoms may indicate the need for a root canal. The procedure involves local anesthesia, cleaning, and filling the tooth's root canal. While root canals have an unfair reputation for pain, most discomfort subsides within 72 hours. Costs vary but can prevent the need for extractions. Success rates are high at approximately 95%, with proper post-treatment care. Myths about pain, cost, and recovery often overshadow the benefits of this essential dental procedure.
The prospect of undergoing a root canal for the first time can be intimidating. In situations where a standard filling cannot save the tooth, a root canal can provide a relatively quick and painless solution.
Regarding Root Canal
Do I require a root canal procedure or endodontic treatment?
If you are experiencing severe tooth pain, extreme sensitivity, tooth discoloration, swollen gums, a recurring abscess on the gum line, or a fissure in a filling, or if you have sustained a traumatic injury to your teeth, you may require a root canal to save your tooth. If your dentist believes you are likely to need a root canal, they will take an X-ray and may test for temperature sensitivity; they may also perform comprehensive imaging. If you have an abscess, your dentist may prescribe antibiotics to treat the infection before commencing treatment, or he or she may recommend a root canal.
If I require a root canal, what is the next step?
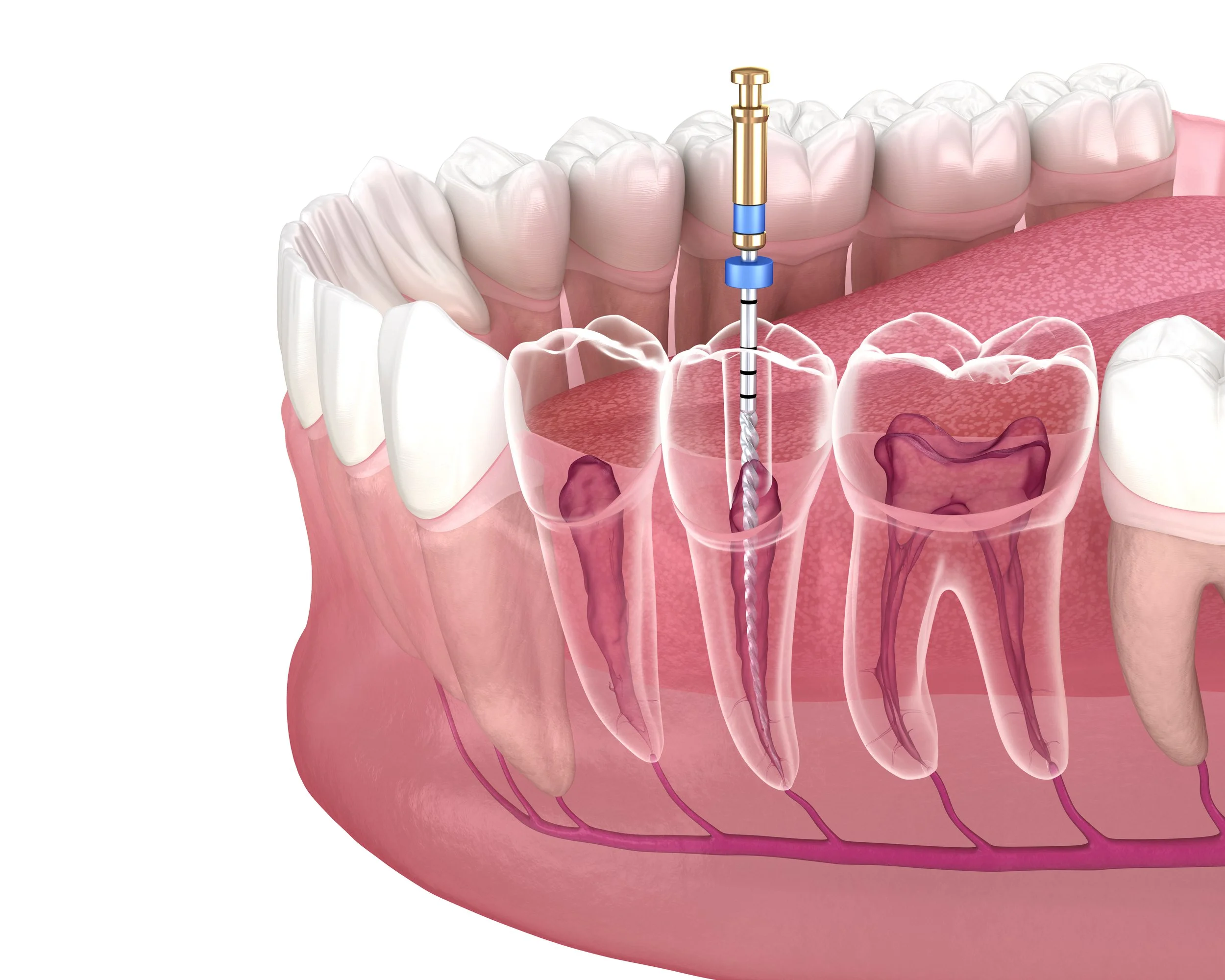
It is essential that you comprehend the root canal procedure, the risks and benefits of the treatment, as well as the treatment's complexity. Root canal treatments are now specially registered with the GDC, and in some cases, your dentist may advise you that a referral to a dentist with a special interest in root canals or endodontics is necessary to ensure long-term success and provide the most effective treatment. Local anaesthesia will be administered to ensure that your root canal treatment is painless. A rubber dam will be inserted around the tooth to maintain a dry environment. An access hole will be drilled, and then decayed nerves and detritus will be removed with files. Then, the root canal will be filled with a polymer compound. Then, a temporary filling may be placed, or in some cases, the permanent filling may be completed at the same appointment.
My root canal treatment will be painful?
Root canal treatment has an unjust reputation for being painful, primarily because patients typically discover they need one after experiencing excruciating tooth or gum pain. As local anaesthetic will be used throughout your treatment, you will experience minimal discomfort at most. 24–72 hours of soreness and discomfort are common following endodontic treatment.
How much does the treatment of a root canal cost?
For the price of a root canal, please visit our website's fee page HERE. In many cases, a root canal can prevent the need for an extraction, and if you take good care of your teeth and tissues after the procedure, root canal treatment can last a lifetime with routine maintenance and check-ups. Please note that following a root canal, you will need a restoration such as a filling or crown. In addition to the cost of root canal, the cost of a filling or crown will be added.
What is the rate of success for root canals?
95% approximately. In extremely uncommon instances, we may discover additional infection in the root after performing a root canal and need to administer additional treatment. In extremely rare circumstances, a root canal may not be able to save the tooth. However, as a treatment with a success rate of 95% and durability for the majority of patients, a root canal is typically an excellent method to avoid extraction. Our opinion is that root canals should be performed by a practitioner with postgraduate experience in this discipline. Treatments and technologies have progressed, increasing the success rate of root canals.
What should I do after the treatment of my root canal?
After your treatment, you may desire to take an over-the-counter pain reliever, such as Aspirin or Ibuprofen, for minor pain or sensitivity. Ensure that you finish any antibiotics prescribed by your dentist and that you continue to brush and floss as usual. Long-term vigilance with brushing and flossing is essential for maximising the effectiveness of root canal therapy. If properly maintained, a root canal can last a lifetime. In the past, patients were typically told that a root canal would last between 8 and 10 years, but we'd add that the longer you want your root canal to last, the better you must care for your teeth and gums! Not smoking, flossing and scrubbing your teeth religiously, and visiting your dentist and hygienist on a regular basis will all contribute to the longevity of your root canal. According to research, all post-root canal procedures should include a crown inlay and post.
Is a root canal a very long procedure?
Root canal procedures can take between two and three hours, depending on their complexity. We may be able to complete your root canal in a single appointment, which will take approximately 90 minutes, but root canals are technically challenging, so time must be taken to achieve the best results.
What are the most prevalent root canal treatment myths?
Root canals are an excruciating procedure. Yes, if you require a root canal, you may arrive at the clinic in agony, but this should subside once we begin treatment! Patients frequently report that the relief they experience once root canal therapy begins and we can stop the tooth and gum pain they've been experiencing is immense, and that root canal therapy itself should be painless.
The cost of root canals is high. They are more expensive than standard composite fillings, but significantly less expensive than dental implants, and if you detect your dental issues early, a root canal may prevent you from needing an implant in the future. A naturally saved root canal is always preferable to an implant, and while the prospect of spending up to three hours in the dentist's chair may be daunting, it's worth it to be pain-free and save your tooth!
That root canals are time-consuming. We may be able to complete your root canal treatment in a single visit, but even if it requires multiple visits, it's a surprisingly quick and effective method to save your tooth!
Root canals have a lengthy recovery period. Similar to after having a filling, you may experience some sensitivity, but this should subside within two days. Additionally, we recommend biting a little more gently on the treated tooth for the next day or so, and Ibuprofen can be consumed. Aside from this, there is virtually no recovery period following a root canal. Just be sure to brush and floss thoroughly, and business as usual will resume after your procedure.
That root canals are not durable. We will provide you with the highest conceivable standard of care. Then the floor is yours. If you take good care of your teeth after root canal therapy, root canals can last for many years. Like anything else, root canal treatment may appear to be costly, time-consuming, and intimidating, but if performed by the right practitioner with the right experience, root canal treatment should be pleasurable and successful!
All There to Know About Dental Implants: A Patient Guide
A dental implant is an artificial tooth root that is typically composed of titanium. When applied with skill, they provide a highly reliable treatment. The primary objective of implant placement is to obtain immediate, intimate contact with the surrounding bone. Over time, additional bone growth on the implant surface improves the implant's stability.
All There Is to Know About Dental Implants : A patient guide
In modern dentistry, dental implants have become the treatment of option for missing teeth.
What exactly is an implant?
A dental implant is an artificial tooth root that is typically composed of titanium. When applied with skill, they provide a highly reliable treatment. The primary objective of implant placement is to obtain immediate, intimate contact with the surrounding bone. Over time, additional bone growth on the implant surface improves the implant's stability.
In order to support replacement teeth, dental implants typically feature an internal screw thread or post space that permits the attachment of a variety of components. Once in place, these components provide long-lasting support for crowns, bridges, or removable dentures.
Who can receive dental implants?
Dental implants are appropriate for the majority of healthy adults. They can only be used once the jawbone has ceased growing, so they are typically not used on children. Habits such as excessive drinking or smoking can increase the number of complications associated with initial healing and may be detrimental to the gum and bone surrounding each implant in the long term. Smoking should be reduced or best still given up altogether. However, each case is unique, and if you have any medical issues, you should consult with one of our implant specialists prior to beginning treatment; in only a few instances do health issues completely preclude the use of dental implants.
Dental implants are appropriate for the majority of healthy adults.
How will you determine if you are a candidate for implants?
During your initial consultation, one of our specialist will determine whether implant treatment is feasible. We discuss your options and conduct an examination of your mouth and remaining teeth to determine the nature and extent of any existing dental issues. Typically, x-rays will be obtained and dental models will be fabricated so that these can be examined after your appointment. These x-rays and models will be used to determine the optimal position for an implant, the number of implants required to fill the gap, and the available bone grade and volume.
Establishing excellent oral hygiene is a crucial step in any treatment plan. At this initial consultation, you will be informed of which problems are essential and what treatment is necessary to stabilise any gum or tooth issues.
Must you maintain a wholesome mouth?
When you inquire about dental implants for the first time, it is frequently in response to ongoing dental issues or the recent loss of teeth. Before implant treatment, it will often be necessary to understand and treat the underlying cause of these issues.
If you have poor breath, loose teeth, or excessive bleeding, especially when your teeth are professionally cleaned, you may have gum disease.
Gum disease (periodontal disease) is a leading cause of bone loss, making dental implant treatment more difficult, but not impossible.
How lengthy is the treatment?
For routine cases, the duration between implant placement and the placement of the first tooth/teeth can range from three to six months. The availability of higher-quality bone can be used to reduce treatment time, whereas inferior bone requires more time and care, which can extend treatment times beyond six months.
What should you understand before beginning treatment?
You will receive a written summary of your discussion regarding treatment planning, emphasising your current dental condition and any alternatives to dental implants. This summary also provides an overview of the anticipated treatment stages and provides an estimate of the expected duration, number of implants, and cost. There may be additional issues unique to your case, and they will be addressed accordingly.
How long do implants typically last?
Once the implants and surrounding soft tissues are deemed to be healthy and the new teeth are deemed to be comfortable and properly aligned, the quality of your oral hygiene and willingness to attend regular maintenance reviews will have the greatest impact on their longevity.
Similar to neglected natural teeth, implants will develop a layer of hard and porous deposits (calculus and plaque) if they are not properly cared for. These deposits, if left untreated, can cause gingival infection, bleeding, soreness, and general discomfort. Implants could be said to have the same longevity as natural teeth. Implants that are well-maintained and placed in sufficient bone can potentially last a lifetime if cared for properly. However, just as you would anticipate traditional crowns, bridges, and fillings to require occasional restorations or replacements, implant-supported teeth may also require similar maintenance over time.
How many teeth can dental implants support?
Dental implants can be used to replace a single tooth or an entire arch of teeth. Dental implants can support all prevalent forms of tooth replacement, such as bridges and dentures.
If you are missing a single natural tooth, one implant will typically suffice to provide a replacement. However, larger spaces created by two, three, or more missing teeth may not require one implant per tooth; the precise number of implants will depend on the grade and quantity of bone at each potential implant site.
Patients with a propensity of clenching or grinding their teeth (bruxism) may be at risk of implant overload. Bruxism occurs during sleep for most individuals, so they are typically unaware of it. The most common clinical indications of bruxism are excessively worn or flattened teeth, chipped enamel edges, and/or the frequent breakage of filling fragments. During treatment planning, the effects of bruxism must be considered, and they can be compensated for by placing additional implants, selecting appropriate restorative materials, and providing a nighttime bite guard to secure the new teeth. This will be covered in your initial consultation and treatment plan.
Implant retained prostheses
What is the therapy?
Using dental implants to anchor removable prostheses is a significantly more effective method than using adhesives, pastes, or powders. With only two implants or four mini implants in each jaw, dentures can be clipped into position and held securely, but are simple to remove for cleaning and sleeping. Implants also provide a number of aesthetic advantages, including the preservation of bone in the jaw and the maintenance of facial structure, as well as the restoration of lost lip support to reduce wrinkles around the mouth. Approximately 15 minutes of the 90-minute procedure are devoted to actual surgery. It is a quick and economical alternative to a complete arch of dental implants.
What alternative treatments are available?
Implant-retained dentures are a significant improvement over traditional removable dentures, which are inconvenient, sometimes uncomfortable, and restrict your diet. Full arch dental implants are an even better alternative to removable dentures; we are one of the few practises in East Anglia with the expertise to conduct this procedure. It's a life-altering, permanent solution.
Is it essential to replace an entire set of lacking teeth?
Multiple tooth loss can have a profound effect on one's quality of life. In addition to having a significant influence on your ability to speak and eat, it can also alter your appearance. Without teeth to support the lips and cheekbones, wrinkles develop more quickly and the cheeks become hollow. Many individuals with this type of tooth loss believe they appear older than they are, which can be detrimental to their self-esteem.
A summary of the implant procedure
Typically, implant treatment consists of several phases that occur over a period of three to nine months. Although there are numerous implant treatment methods, a typical procedure typically involves the following:
Assessment and planning for treatment:
At the initial consultation, after a thorough discussion of all potential alternatives, we will determine whether implant treatment is feasible. If necessary, x-rays will be obtained and models of the teeth will be created. Then, a written treatment plan detailing the treatment sequence and associated costs will be created.
Implant placement:
Implant implantation is a relatively straightforward minor surgical procedure that can be performed in a dental office under sterile conditions.The procedure is performed under local anaesthesia and, if necessary, sedation. If, during evaluation, it is determined that the underlying bone is deficient, there are several options for bone regeneration. Depending on the needs, bone regeneration is typically performed at the same time as implant placement.
Transition period:
It can take between six weeks and six months for implants to integrate with a patient's bone. During this period of integration, temporary dentures or bridgework may be worn as needed. In certain instances, temporary teeth can be affixed to the implants in a procedure known as "immediate loading" while the implants integrate.
The Recuperative stage:
Once implants are incorporated, they can be restored with a variety of new teeth (definitive restorations) including a single crown, small or large bridge, or removable overdenture. We collaborate closely with a laboratory that creates these permanent restorations.
Maintenance:
Following conclusion of implant treatment, the patient must clean the new teeth (restorations) according to the instructions. A dental hygienist may also provide guidance on the care and upkeep of restorations and natural teeth. Regular visits to the dentist are required so that the health of the soft tissues, bone levels, and restoration can be evaluated.
How can you determine if you have sufficient bone for dental implants? Normal dental x-rays display a great deal of detail, but only in two dimensions. From these views, it is typically possible to determine the height of available bone for implant placement; however, sometimes more advanced imaging techniques are required to determine the equally crucial bone breadth.
Dental CBCT Scans – there are now a number of sophisticated x-ray techniques that enable a three-dimensional examination of the jawbone. CBCT (cone beam computed tomography) scans are the most precise and widely available. Images obtained by CBCT scanning will typically display all of the necessary bone information, including quantity and quality, but most importantly the presence of structures that must be avoided.
What may result in bone loss?
When a tooth is lost or extracted, a significant portion of the bone that once encompassed the remaining root may be lost. This loss is referred to as "bone resorption" and can be especially rapid during the first few months. Despite the fact that the rate and quantity of bone resorption is highly variable between individuals, it will always occur to some degree unless special precautions are taken to mitigate its effects.
Many patients report that their dentures gradually become looser and no longer fit as well as they once did. Initially, the observed worsening of denture fit is a result of the increased rate of bone loss following tooth extractions.It is the direct effect of gnawing forces that causes the gradual deterioration of supporting bone over time. Therefore, the longer prostheses are worn, the less available bone there is for dental implants.
What anatomical structures must be avoided during dental implant placement?
As long as the implants remain within the bone that once supported your natural teeth, there are no significant risk areas in the upper mandible. If you are missing upper back teeth, you can be shown the contour and location of the area above the roots (maxillary sinuses). Since the maxillary sinuses are visible on the majority of x-rays, they are generally avoided.
The 'inferior dental nerve' is the most vital anatomical structure to avoid in the lower mandible. This nerve begins behind the wisdom teeth, travels under the back teeth (molars), and emerges on the epidermis of the face where the middle teeth (premolars) are or were. This is the reason why a normal dental anaesthetic numbs the lip even when the needle is inserted in the very back of the mouth. If this nerve is irritated or damaged during dental implant implantation, it can result in temporary or permanent numbness or altered sensation. This is an uncommon but significant complication.CBCT scans are typically the most accurate method for pinpointing the location of this nerve, allowing implants to be implanted with confidence. CBCT scans are more expensive than standard dental x-rays, but the information they provide is often invaluable for complex treatment planning and determining the location of vital anatomical structures. If a tooth is inadvertently damaged by the implantation of a nearby implant, any resulting issues can typically be treated with root canal therapy, in which the tooth's nerve is removed.
Can dental implants preserve bone?
This is one of the most essential characteristics of dental implants. Once in place and supporting teeth, daily functional forces (eating, smiling, speaking) stimulate the adjacent bone, causing it to become denser and stronger. As with all things, there are limitations to the amount of labour an implant can perform. We will discuss this in greater depth as it pertains to your specific situation.
Can replacement teeth be worn while undergoing implant treatment?
If the teeth being replaced by dental implants are in a highly visible area of the mouth, it is probable that you will need to have some teeth present during the procedure. This can be accomplished in a variety of methods, ranging from simple plastic dentures to removable bridges. If replacement teeth are used during treatment phases, it is vital that they do not exert uncontrolled pressure on the implants. You should anticipate a number of visits for minor adjustments to any temporary teeth after the implants are inserted and before they are activated. They might not be as visually appealing as your final restoration.
Are dental implants compatible with natural teeth?
Dental implants are routinely inserted adjacent to natural teeth, and this procedure is generally very safe. The only exception to this rule would be if the natural root was extremely curved or inclined in the proposed implant path. This could cause the implant to damage the root, but this is typically avoidable through meticulous pre-operative planning.
Are the replacement molars fused together?
When numerous implants are inserted, they are typically connected in the same manner as a bridge supported by natural teeth. When teeth supported by implants are joined together, they are mechanically sturdier than the sum of their parts.
If sufficient implants are available, it is frequently simpler and just as effective to construct several smaller bridge sections, each supporting a few teeth. The overall effect in the mouth is identical, and if you ever need to repair one of the minor sections, this can be accomplished much more easily. Again, the quality of the bone, as well as the number and placement of the implants, will determine which option is most suitable for you.
Is it unpleasant when implants are inserted?
The majority of patients will be familiar with the anaesthetics used in routine dentistry and will be aware of their efficacy. The same anaesthesia is used to insert implants. Depending on the complexity of your case, the procedure could last anywhere from 30 minutes for a single implant to several hours for complex bone augmentation and implantation of multiple implants. Expect some minor swelling and occasional discoloration after surgery. For the majority of patients, fundamental over-the-counter pain relievers will suffice for several days. If you continue to experience discomfort, contact your healthcare provider, who can prescribe a stronger medication.
Generally, healing is uncomplicated, and sutures are removed within a week to ten days. During the initial few days, you should disclose any unanticipated pain or swelling so that it can be evaluated. Always seek advice when in doubt, as early detection of a problem often leads to a simplified solution. You may also be prescribed antibiotics and asked to perform some basic procedures, such as rinsing your mouth with salt water or an antiseptic mouth rinse. It is essential that you follow these directions.
If the implant surgery will require a long time, is sedation an option?
Although it is relatively simple to provide effective pain management during surgery, the majority of patients will be apprehensive. There is no need to suffer in silence, as there are numerous highly effective ways to attain a state of relaxation.
Conscious sedation – For more complex procedures, it may be recommended that you have a more regulated method of relaxation and comfort during the surgical phases. This is known as 'conscious sedation' and is distinct from a anaesthetic because you are awake enough to respond to simple instructions that may be helpful to the surgeon; however, you will recall almost nothing of the treatment phase. It is especially advantageous for procedures lasting more than an hour that do not require hospitalisation; this is likely the case for the majority of dental implant treatments.For routine "conscious sedation," a sedative is administered via an arm or hand vein for the duration of the procedure. An anesthesiologist continuously monitors your pulse rate and oxygen levels during this extremely safe procedure. A standard dental local anaesthetic is injected around the proposed implant sites under conscious anaesthesia. By the time the dental anaesthetic is administered, the anaesthesia has already taken effect, so most patients do not recall this phase. For procedures requiring oral or conscious anaesthetic, you may be asked to refrain from eating or drinking for at least four hours prior to surgery, and you will be required to make arrangements for an adult to drive you home. Additionally, you will be instructed not to operate any apparatus for at least 24 to 36 hours.
What can be done if there are insufficient bones?
Up to this point, we have covered the fundamentals of routine implant placement. This has included the initial examination and diagnosis, special x-rays such as CBCT scans, anaesthetic during surgery, and what to expect following the placement of implants. However, for some individuals, bone loss following tooth extraction or loss prevents the placement of an implant. There are actions that can be taken if this occurs:
It is possible to increase the height of available bone in the upper jaw above the back molars by creating new bone in the sinus.This process is known as a "sinus augmentation." Without the widespread success of this technique, numerous patients would be unable to receive dental implants in a region of the mouth where tooth loss is so prevalent.
There are numerous methods for adding bone, but one of the simplest is to remove a piece of bone from another location and attach it as a "onlay graft" to a deficient area. The new piece of bone will gradually fuse with the underlying bone, and an implant can be implanted in a more favourable position once it has healed and matured.
Where can additional bone be obtained?
Bone can be harvested from a variety of locations, but most commonly from the back of the lower mandible or the chin. Occasionally, it is extracted from the hip or tibia. When using your own bone to create new bone in another area of the mandible, you will experience discomfort at both the donor site and the surgical site. As your own bone is typically regarded as the 'gold standard,' many people feel that the additional discomfort is well worth it.
Alternatives to your own bone for augmentation There are other sources of bone, such as bovine (derived from cows), porcine (derived from pigs), and synthetic materials that have been specially processed to make them acceptable for use in humans, for those who prefer an easier but slightly slower solution. All of these materials, including your own bone, are merely scaffolds into which new bone will grow in a few months in preparation for dental implant placement.
It can take anywhere from three to twelve months for new bone to be suitable for dental implants. Do not rush to advance to the next stage. A larger quantity of bone will take longer to mature than a smaller quantity. Each surgeon will have a preferred technique for producing new bone. Many of them will additionally employ a technique known as "guided tissue regeneration." By placing a barrier material between slow-moving bone cells and the fast-moving cells of the soft tissues lining the mouth, this technique allows slower-moving bone cells time to occupy a space. This is a "resorbable barrier" that will dissolve spontaneously after a few months of performing its function.
Does bone augmentation impact treatment duration?
If you require bone augmentation, it may lengthen the duration of your treatment; however, when performed successfully, it will significantly enhance the outcome of the implant(s) placed. When used in the front of the mouth, it can also enable the construction of much more aesthetically pleasing results.
Regardless of the method selected to increase bone density, the time, effort, and expense are generally worthwhile.
How do you care for your implants?
To increase the longevity of your implants, it is imperative that you maintain excellent oral hygiene. Cleaning your implants is straightforward. For the majority of implant-supported teeth, you will be able to brush and floss around each supporting implant just as you would around natural teeth and tooth-supported bridges. Maintaining excellent oral hygiene may require special floss, interdental toothbrushes, and other cleaning aids in some areas.
If you wish to maintain optimal implant health, it is reasonable to anticipate that some daily maintenance procedures will be more complex than those performed around your natural teeth, and that you will need to devote more time than in the past.
During the first few months following implant placement, your dentist may request that you visit them more frequently; however, once they are satisfied that your treatment is proceeding according to plan, your ongoing dental care will be comparable to that of a patient with natural teeth.
What options exist if an implant fails?
The average success rate for dental implants is approximately 96%; you should discuss how the loss of an implant could affect your treatment plan. A dental implant can fail for a variety of reasons, including smoking, poor oral hygiene, and systemic disease. In these particular high-risk groups, one would anticipate a much higher failure rate. If an implant does not integrate well with the surrounding bone, it will ultimately lose its ability to support replacement teeth and become loose. Commonly, a failing implant does not cause discomfort, and if there are sufficient residual implants, it may not be necessary to replace it.
It is essential to discuss the potential complications that may arise.
Various implant procedures
One-stage implant – The implant is inserted into a fresh, healing, or healed extraction site where the original tooth was extracted, and is immediately visible above the gum. This technique has the advantage of not requiring a second surgical stage to expose the implant. Typically, the implant will not be able to sustain a tooth for several weeks or months.
This is the first stage of a two-stage implant, in which the implant is inserted into a fresh, healing, or healed extraction site and then concealed by a layer of gum tissue. At the second stage, weeks or months later, the implant is uncovered and components are added, bringing it to the surface of the gum so that a new tooth can be attached.
Same-day implants necessitate meticulous planning prior to the actual day of surgery. A few hours after the placement of multiple implants, a full arch of temporary or permanent teeth can be affixed. If temporary dentures are used, they are typically replaced with a permanent bridge after a sufficient period of healing. Not all patients are appropriate candidates for this method of treatment.
In this procedure, a tooth is extracted and an implant is placed promptly into the extraction site. Depending on the local bone and soft tissue conditions, implant surgery may be performed in one or two stages. Not all patients are candidates for this treatment.
Immediate implant placement and early loading – This is dissimilar to immediate implant placement. It is essentially a one-step procedure in which the implant is inserted into a fresh, healing, or healed extraction site and a replacement tooth is attached at the same appointment. This first tooth will typically be kept out of direct contact with opposing teeth for more than three months, following which it will be restored. This procedure is more prevalent in areas of the mouth where aesthetics play an essential role. Again, this approach is not suitable for all patients.
Frequently asked questions:
Will I be able to consume my favourite foods afterwards?
Patients should be able to consume a normal, nutritious diet with little to no difficulty upon completion.
What are the costs associated with implant treatments?
The price can vary based on the required level and extent of treatment. A written treatment plan therefore explains and confirms the total cost.
How much time will it take?
Implant treatment typically requires multiple appointments over the course of several months. In certain instances, implant procedure can be completed much more quickly.
How lengthy is its duration?
Regular dental hygiene and regular checkups should ensure that implants last for many years after treatment is complete.
Am I too elderly to receive implants?
There is no upper age limit for patients undergoing implant treatment, so long as they remain in reasonable health.
Is the procedure painful?
Patients are frequently astonished by the lack of pain they experience during and after implant procedures.
Glossary:
-Abutment
Abutment is the component that connects the implant to the permanent tooth restoration.
-Barrier membrane
A membrane that is draped over a bone defect or bone implant to prevent the infiltration of soft tissue, which could compromise the healing process.
-Bone augmentation
This is the insertion of natural or synthetic bone material in a deficient area of natural bone. This procedure may be performed concurrently with implant implantation, or as a separate procedure prior to implant placement.
-Bone resorption
Resorption of bone is the loss of bone height and/or width in the upper or lower mandible. This process continues throughout life, but is accelerated in areas where teeth have been lost.
-Bridge
A bridge is a method for replacing one or more missing teeth with artificial teeth that are bonded to adjacent natural teeth or dental implants. Bridges may be glued in position (adhesive bridges) or supported by crown preparations (conventional bridges) and constructed from a number of different materials.
-Bruxism
The act of clenching or grinding one's teeth when not chewing.
-Calculus
Sometimes referred to as tartar, tartar is a hard deposit that forms on teeth. Calculus is the result of the calcification of debris around the teeth, and it can be avoided by practising meticulous oral hygiene. Once calculus has formed, it is difficult to eradicate, and requires the services of a dental therapist or hygienist in most cases.
-Absolute arch
A complete arch refers to the teeth of the upper or lower mandible in their entirety.
-Consultation
A dental consultation to evaluate potential treatment options. Appointments may include an examination, x-rays, and photographs, as well as a frank discussion and explanation, if necessary.
-Crown
Crowns can be manufactured from a variety of materials, including porcelain, porcelain fused to metal, and gold. The majority of crowns that are not visible in the mouth are white in pigmentation.
-CBCT scan
Cone Beam Computed Tomography is a sophisticated x-ray technique that generates three-dimensional images of the mandible. Due to their three-dimensional nature, these images can only be observed on a computer screen.
-Definitive refurbishments
The definitive restoration refers to the ultimate implant-supported crown, bridge, or denture fabricated during the treatment process. The restoration will require routine maintenance and may require replacement.
-The administration of dental anaesthetics
Anaesthesia (Greek: ) means without sensation, which includes pain. The majority of dental anaesthetics are administered via injection into the affected area. Rarely, procedures may be performed while you are unconscious; this is known as a general anaesthetic.
-Dental implant
An implant is an artificial "tooth root." The majority of implants are composed of metal, with titanium or titanium alloys being the most prevalent. Implants are surgically inserted into the jawbone in order to support crowns and bridges or to stabilise dentures.
-Dentures
Dentures are removable, custom-made replacement teeth. Typically, they are composed of acrylic or acrylic and cobalt chromium.
-Extraction
Extraction of teeth is the removal of teeth.
-Extraction position
The space left after tooth extraction.
Effective implantation
A functioning implant is one or more implants that are capable of supporting a dental restoration, such as a crown, bridge, or denture, and biting.
-Therapeutic tissue regeneration
A procedure that promotes the regeneration of soft tissue (gums) and may be used to improve the aesthetics around teeth or crowns.
-Gum disease
Soft tissue disease surrounding teeth. Gingivitis is the common name for gingival inflammation; it is a response to the deposition of plaque and, in most cases, can be treated with rigorous oral hygiene.
-Periodontal disease
Gingivitis can develop into periodontitis, a more severe form of gum disease, if left untreated. Periodontitis causes bone loss and can threaten the survival of a tooth or teeth.
-Immediate loading
Providing a temporary crown or bridge concurrently with implant implantation. Not all patients are appropriate candidates for this treatment.
-Inferior dental nerve
This nerve, sometimes known as the inferior alveolar nerve, travels through a bony canal in the lower jaw and provides sensation to the lower teeth, before emerging from bone as the mental nerve, which provides sensation to the lower lip.
-Combination toothbrushes
A small interdental brush with typically a single tuft of filaments. This can be used as an alternative to dental floss for cleansing between teeth and around implants.
-Maximum sinus
A hollow, air-filled space located just above the upper premolars. This varies in size from person to person and grows throughout one's lifetime.
-Molars
The upper and lower third molars on both sides of the mandible.
-Onlay anastomosis
When bone is taken from another area of the body, such as the hip (rarely), jaw, or behind the molars, and grafted to a deficient area.
-Osseointegration
Osseointegration is the bonding or fusion of an implant and bone, which typically takes several weeks to months.
-Plaque
Plaque is a soft, sticky, colourless film of bacteria that forms continuously on teeth and gums and can harden into calculus if not removed daily by practising good oral hygiene (brushing, flossing, etc.).
-Premolars
The two teeth located on both sides of the mandible in front of the molars.
-Reline procedure
During a relining procedure, a soft or firm material is used to correct the fitting surface of a denture following an extraction or surgery.
-Removable overdenture
A removable denture that is supported by implants but can be removed by the patient for cleansing.
-Restorations
The restoration may consist of a filling, a crown, a bridge, or a denture. It restores the tooth or teeth to full functionality.
-Rejuvenating phase or appointment
This phase follows the surgical phase of the treatment plan, typically a few weeks to a few months after a sufficient degree of recuperation. In the majority of instances, this will involve obtaining impressions so that the technician(s) can fabricate the definitive restoration.
-Sinus augmentation
A surgical procedure in which bone regenerative material is inserted into the sinus to stimulate the formation of new bone in order to enhance the available bone height for implant placement.
-Sterile conditions
In this context, sterility refers to the absence of bacterial contamination. We can never achieve absolute sterility, but we must always strive to achieve as near as possible to a sterile working environment. This includes the use of autoclaves to sterilise all nondisposable instruments as well as drapes and robes to isolate working surfaces and personnel.
-Titanium
This biocompatible metal is used to manufacture implants. Titanium has been utilised for decades in medical procedures, including hip replacements.
-Treatment scheme
A report outlining the patient's dental implant procedure, including the proposed treatment timeline and expenditures. The purpose of this guide is to provide an overview of standard dental implant treatment. Each individual's treatment plan for dental implants will be customised by Norfolk Dental Specialists in terms of cost, duration, and method of care delivery.
How Bite Splints and Dental Occlusion Adjustments Can Help with Relief from Ear Tinnitus and TMJ Pain?
Living with ear tinnitus and TMJ pain can be incredibly challenging, affecting both our physical and emotional well-being. However, as a dentist, I am here to shed light on a lesser-known solution that can provide relief for these conditions. By addressing occlusal interferences and utilising custom-made bite splints, we can effectively reduce ear ringing and alleviate TMJ pain, ultimately improving your quality of life.
Living with ear tinnitus and TMJ discomfort can be extremely difficult and detrimental to our physical and mental health. But as a dentist, I'm here to highlight a less well-known treatment that helps alleviate these symptoms. We can successfully minimise ear ringing and relieve TMJ pain by correcting occlusal interferences and using personalised bite splints, thereby enhancing your quality of life.
Recognising the Relationship:
It is impossible to emphasise the complex relationship between tooth occlusion and ear tinnitus or TMJ pain. Occlusal interferences, which lead to imbalances in the jaw joint, might be the result of misaligned teeth, a bad bite, or persistent grinding and clenching. These imbalances can result in ear tinnitus and TMJ pain, which can cause discomfort, decreased functionality, and a general decline in wellbeing.
Occlusal Adjustments for Relief:
Making occlusal modifications is one of the most important strategies for dealing with these problems. A qualified dentist can find interferences and imbalances by thoroughly analysing your teeth's alignment and evaluating your bite. We can eliminate tension on the jaw joint and the resulting symptoms of ear tinnitus and TMJ pain by making exact changes to your dental occlusion.
Customised Bite Splints:
When occlusal modifications alone may not be enough to relieve pain, using bite splints can be quite helpful. Bite splints, commonly referred to as removable appliances, are made-to-measure tools used to realign the jaw and offer a secure, comfortable position for biting. These splints not only relieve pressure on the jaw joint but also guard the teeth from wear and tear caused by clenching and grinding. Patients who use bite splints on a regular basis report less ringing in their ears and TMJ pain, as well as enhanced jaw mobility and better oral health.
Getting Professional Assistance:
Consult with a dental expert who specialises in occlusion and temporomandibular joint issues if you are experiencing ear tinnitus, TMJ pain, or TMJ clicking. Our knowledgeable staff at Clinic For Implant & Orthodontic Dentistry, located at 7 Chapel Road in Worthing, BN11 1EG, is committed to offering these patients individualised attention and successful treatments. To take the first step towards receiving the assistance you need, schedule a consultation right away.
Despite the difficulty of dealing with ear tinnitus and TMJ pain, relief is possible with the correct dental treatment. An expert dentist can significantly lessen ear ringing and TMJ symptoms by resolving occlusal interferences and deploying bespoke bite splints. Reach out to our dentist office right now to start your journey towards a better, pain-free life and don't let these conditions hold you back.
What is Root canal treatment?
If you are experiencing severe tooth pain, extreme sensitivity, tooth discoloration, swollen gums, a recurring abscess on the gum line or a fissure in a filling, or if you have sustained a traumatic injury to your teeth, you may require a root canal to save your tooth.
The prospect of undergoing a root canal for the first time can be intimidating. In situations where a standard filling cannot save the tooth, a root canal can provide a relatively quick and painless solution.
DO I REQUIRE A ROOT CANAL PROCEDURE OR ENDODONTIC TREATMENT?
If you are experiencing severe tooth pain, extreme sensitivity, tooth discoloration, swollen gums, a recurring abscess on the gum line or a fissure in a filling, or if you have sustained a traumatic injury to your teeth, you may require a root canal to save your tooth. If your dentist believes you are likely to need a root canal, they will take an X-ray and may test for temperature sensitivity; they may also perform comprehensive imaging. If you have an abscess, your dentist may prescribe antibiotics to treat the infection before commencing treatment, or he or she may recommend a root canal.
IF I REQUIRE A ROOT CANAL, WHAT IS THE NEXT STEP?
It is essential that you comprehend the root canal procedure, the risks and benefits of the treatment, as well as the treatment's complexity. Root canal treatments are now specially registered with the GDC, and in some cases, your dentist may advise you that a referral to a dentist with a special interest in root canals or endodontics is necessary to ensure long-term success and provide the most effective treatment. Local anaesthesia will be administered to ensure that your root canal treatment is painless. A rubber dam will be inserted around the tooth to maintain a dry environment. An access hole will be drilled, and then decayed nerves and detritus will be removed with files. Then, the root canal will be filled with a polymer compound. Then, a temporary filling may be placed, or the ultimate filling may be completed during the same appointment in some instances.
MY ROOT CANAL TREATMENT WILL IT BE PAINFUL?
Root canal treatment has an unjust reputation for being painful, primarily because patients typically discover they need one after experiencing excruciating tooth or gum pain. As local anaesthetic will be used throughout your treatment, you will experience minimal discomfort at most. 24-72 hours of soreness and discomfort are common following endodontic treatment.
HOW MUCH DOES THE TREATMENT OF A ROOT CANAL COST?
For a cost of a root canal please visit our website fee page HERE. In many cases, a root canal can prevent the need for an extraction, and if you take good care of your teeth and tissues after the procedure, root canal treatment can last a lifetime with routine maintenance and checkups.Please note that following a root canal, you will need a restoration such as a filling or crown. In addition to the cost of root canal, the cost of a filling or crown will be added.
WHAT IS THE RATE OF SUCCESS FOR ROOT CANALS?
90% approximately. In extremely uncommon instances, we may discover additional infection in the root after performing a root canal and may need to administer additional treatment. In extremely rare circumstances, a root canal may not be able to save the tooth. However, as a treatment with a success rate of 90% and durability for the majority of patients, a root canal is typically an excellent method to avoid extraction. Our opinion is that root canals should be performed by a practitioner with postgraduate experience in this discipline. Treatments and technologies have progressed, increasing the success rate of root canals.
WHAT SHOULD I DO AFTER THE TREATMENT OF MY ROOT CANAL?
After your treatment, you may desire to take an over-the-counter pain reliever, such as Aspirin or Ibuprofen, for minor pain or sensitivity. Ensure that you finish any antibiotics prescribed by your dentist and that you continue to brush and floss as usual. Long-term vigilance with brushing and flossing is essential for maximising the effectiveness of root canal therapy. If properly maintained, a root canal can last a lifetime. In the past, patients were typically told that a root canal would last between 8 and 10 years, but we'd add that the longer you want your root canal to last, the better you must care for your teeth and gums! Not smoking, flossing and scrubbing your teeth religiously, and visiting your dentist and hygienist on a regular basis will all contribute to the longevity of your root canal. According to research, most post-root canal procedures should include a crown inlay and post.
IS A ROOT CANAL A VERY DELAYED PROCEDURE?
Root canal procedures can take between two and three hours, depending on their complexity. We may be able to complete your root canal in a single appointment, which will take approximately 60 minutes, but root canals are technically challenging, so time must be taken to achieve the best results.
What are the most prevalent root canal treatment myths?
Root canals are an excruciating procedure. Yes, if you require a root canal, you may arrive at the clinic in agony, but this should subside once we begin treatment! Patients frequently report that the relief they experience once root canal therapy begins and we can stop the tooth and gum pain they've been experiencing is immense, and that root canal therapy itself should be painless.
The cost of root canals is high. They are more expensive than standard composite fillings, but significantly less expensive than dental implants, and if you detect your dental issues early, a root canal may prevent you from needing an implant in the future. A naturally saved root canal is always preferable to an implant, and while the prospect of spending up to three hours in the dentist's chair may be daunting, it's worth it to be pain-free and save your tooth!
That root canals are time-consuming. We may be able to complete your root canal treatment in a single visit, but even if it requires multiple visits, it's a surprisingly quick and effective method to save your tooth!
Root canals have a lengthy recovery period. Similar to after having a filling, you may experience some sensitivity, but this should subside within two days. Additionally, we recommend biting a little more gently on the treated tooth for the next day or so, and Ibuprofen can be consumed. Aside from this, there is virtually no recovery period following a root canal. Just be sure to brush and floss thoroughly, and business as usual will resume after your procedure.
That root canals are not durable. We will provide you with the highest conceivable standard of care. Then the floor is yours. If you take good care of your teeth after root canal therapy, root canals can last for many years. In general, root canals that are not performed accurately fail. Remember to inquire honestly about your dentist's experience with root canal treatments. Ask them if they use a microscope and for their assessment of the risks and benefits of the treatment. Root canal treatment may appear to be costly, time-consuming, and intimidating, but if performed by the right practitioner with the necessary experience, it should be a pleasant and successful procedure at Clinic for Implant & Orthodontic Dentistry, 7 Chapel Road, Worthing (West Sussex), telephone number 01903-821822.
A Guide to Wear-Down Teeth: Signs, Symptoms, and Dental Treatments
In this article, we will delve into the causes, symptoms, and available dental treatments for worn-down teeth. Understanding the aetiology of this condition, recognizing its symptoms, and exploring the various treatment options can help you maintain optimal oral health.
Recognising Wear-Down Teeth: Signs, Symptoms, and Dental Treatments
Introduction:
It is my pleasure as a dentist to provide some general information inform about worn-down teeth, their causes, symptoms, and the possible therapies for this prevalent dental condition. Worn-down teeth, sometimes referred to as tooth wear or dental erosion, happen when the enamel, the teeth's protective outer coating, gradually erodes as a result of many causes. Knowing the cause, identifying the symptoms, and getting the right dental care can help stop additional harm and improve your oral health.
Worn-Down Teeth Causes: A number of factors can lead to worn-down teeth, including:
Bruxism:
Teeth grinding or clenching, frequently unintentionally while sleeping, places an excessive amount of pressure on the teeth and causes enamel erosion and attrition.
Acidic Foods and Drinks:
Regularly consuming acidic foods and drinks (such citrus juices and soft drinks) will eventually destroy the enamel.
Brushing Too harsh:
Using a toothbrush with harsh bristles or brushing too vigorously can both lead to enamel damage.
Acid Reflux:
Acid reflux can expose teeth to stomach acid, which erodes the enamel. This condition is known as gastroesophageal reflux disease (GERD).
Certain Drugs:
Drugs that contain aspirin or antihistamines, for example, might produce dry mouth, which reduces saliva flow and makes teeth more prone to wear.
Age:
Over time, natural wear and tear can progressively wear away the enamel, increasing the risk of erosion.
Other Factors:
Chewing on hard things (such ice or pen caps), misaligned teeth, and other underlying medical disorders can also lead to tooth deterioration.
Signs of worn-down teeth include:
The following signs of worn-down teeth include:
Increased Sensitivity of the Teeth:
Worn enamel exposes the underlying dentin, increasing sensitivity to meals that are spicy, cold, sweet, or acidic. Teeth that Look Flattened or Rounded: Enamel loss can give teeth that bite surfaces a rounded or flat look.
Changes in Tooth Colour:
Teeth may seem yellow or discoloured as enamel erodes. Small chips, fissures, or rough edges may appear on worn-down teeth.
Pain in the teeth:
Serious tooth wear may cause pain or discomfort, particularly while chewing or biting.
Dental Procedures for Damaged Teeth:
Depending on the severity of the issue, a number of treatment methods are available for worn-down teeth:
Dental Bonding:
In minor circumstances, dental bonding can be performed to restore the shape, function, and appearance of the afflicted teeth by coating them with tooth-colored resin.
Dental crowns:
Dental crowns may be suggested in cases of more severe tooth wear. These specialised tooth-shaped caps completely encase the tooth, giving it strength, protection, and a more appealing appearance. When the damage is too severe for a conventional filling but does not require a full crown, inlays and onlays—also known as indirect fillings—are employed. They are created in a dental lab, and after that, the tooth is attached to them.
Orthodontic therapy:
If misaligned teeth are a factor in the deterioration of certain regions, orthodontic therapy with braces or invisible aligners may be suggested to rectify the alignment and stop further deterioration.
Nightguards or Splints:
If bruxism is wearing down your teeth, a nightguard or splint can be designed specifically for you to protect your teeth while you sleep and lessen the forces that cause grinding or clenching. Lifestyle Modifications: It's critical to pinpoint and address the root causes of tooth deterioration. Enamel erosion can be stopped by altering diet and dental hygiene practises, cutting back on acidic food and drink intake, brushing correctly, and addressing medical disorders like acid reflux.
Conclusion:
The key to dealing with worn-down teeth is to understand the causes, identify the symptoms, and seek the proper dental care. I advise you to make an appointment with a dentist if you notice any indications of tooth wear. A thorough examination will reveal the full amount of the harm, allowing for the creation of a customised treatment strategy that will restore your smile and safeguard your dental health. Keep in mind that early treatment is essential for avoiding additional issues and preserving a beautiful, healthy smile.
Diet Advise following Full Jaw Implant Surgery.
All-on-4 implant surgery is a treatment option for those with periodontal disease or tooth decay. The procedure involves placing implants in the jaw to support a full arch of replacement teeth. After the surgery, patients can expect some adverse effects, including minimal oozing, swelling, tense jaw and facial muscles, and site-specific pain. These symptoms are temporary and can be managed with over-the-counter pain medication. It is important to rest for the first three to four days, then gradually resume normal activities and exercise.
All-on-4 implant surgery is a thorough and successful treatment for periodontal disease and tooth decay, in cases where an entire upper or lower arches are missing or irreparable. Before the benefits of All-on-4 implant surgery take full impact, you can anticipate certain adverse effects after surgery. Possible symptoms include:
- Minimal oozing
- Swelling
- Tense jaw and facial muscles
- Sore throat and/or trouble swallowing
- Site-specific pain
If you experience adverse effects, they are transient and often subside after one week. Any pain or discomfort can be alleviated with over-the-counter drugs such as Paracetamol, Aspirin, or Ibuprofen.
It is very imortant to rest for the first three to four days. After that period of time, and as tolerated, you may resume normal activities and exercise.
However, dietary limitations last longer. These constraints can be divided into two time categories:
- First three weeks after surgery
- From three to six weeks after surgery
Knowing which foods are acceptable to eat following the surgery are crucial, as they will help you with the following;
- Reduces the impact of any pain and/or swelling
- Promotes a rapid recovery
- Maximise the benefits of your All-on-4 operation
If you already have dietary restrictions due to a medical condition (such as diabetes), you should visit a physician or trained nutritionist for advice.
Blender for soft food diet - after surgery, a blender will be your best buddy.
3 Weeks Post-Surgery: Eating on a Liquid Diet
Your mouth, jaw, and throat are likely to be painful for either a few days or up to three weeks after surgery, however any pain or swelling will progressively lessen. As a result, eating might be unpleasant or challenging. During this time a liquid diet without chewing is required.
Here are some considerations to make during this time period;
- The majority of pain post surgery is felt immediately after the surgery. It may be challenging to open your mouth and swallow. If your jaw feels rigid, making it difficult to open your mouth, try massaging it with an ice pack.
- Liquids can be consumed shortly after surgery. In the first 48 hours, you should only consume cool liquids. If you intend to consume something hot, do so until after the anaesthetic has worn off and all bleeding has ceased. It is best to avoid hot or spicy liquids until the third or fourth postoperative day.
- Hydration is key! It's important to consume a great deal of fluids, but in tiny quantities and often throughout the day. Once the anaesthetic has worn off and you feel comfortable enough, you should consume clear fluids shortly after surgery. Fluids will restore and maintain the tissue's moisture for optimal healing, regardless of whether there is drainage following the procedure.
- You will experience hunger as a result of consuming just liquids and avoiding solid foods for the first three weeks following All-on-4 implant surgery. In addition, optimal nutrition is necessary to avoid illness and accelerate recovery. Ensure that the fluids you consume during the day are nutrient-rich and that you consume them often. Given that you have just undergone oral surgery, it is expected that your intake would be lower than usual. However, you must bear in mind that nourishment is essential to healing, and without it you may experience a delay. Following is a list of foods that can be consumed during the first one to two weeks following surgery.
Important - do NOT use a straw when consuming liquids or liquidised food. The sucking movement might loosen blood clots, causing more bleeding and delaying the healing process.
What foods may I consume during this time?
There are numerous liquid foods that can be consumed during the first three weeks following All-on-4 implant surgery. The following are examples of consumable liquids;
- Soup broths (bouillon - beef, poultry, and vegetable)
- Creamy soups (without solids)
- Coconut liquid
- Kefir drinks
- Fruit juices
- Tea/coffee
- Warm cocoa
- Milk, including all forms of cow milk, from fat-free to whole
- Milk derived from nuts or peas
- Milkshakes
- Yogurt drinks
- Meal substitute shakes
- Protein shakes
- Smoothies
- Sodas
- Gelatine (e.g. Jelly)
- Custard
- Ice cream
- Frozen fluids, like fruit ices or popsicles
- Frozen yoghurt
When consuming milkshakes, yogurt drinks, fresh fruit jucies, smoothies and protein shakes, the consistency should be light enough for easy sipping. As the days pass and you feel you can stomach it, you can consume heavier shakes.
When you need to increase your calorie intake, put the following foods in your shakes:
Whites of powdered eggs, milk powder products, instant breakfast mixes (e.g., instant oatmeal), butter, margarine, or oil, sugar, syrup, or honey, or brewing yeast.
Sample Menu for first three Weeks After Surgery
Following is an example of a one-day menu for a fluid diet immediately following All-on-4 surgery. It is vital to note that you should have snacks to ensure that you receive the necessary nutrients and calories for recuperation.
Breakfast
- Fruit juice or smoothie
- Cup of tea or coffee
- Yogurt
- Glass of water
Breakfast Snack
- Glass of fruit juice
- Glass of water
Lunch
- Meal replacement drink
- Cup of broth
- Jelly
- Glass of water
Dinner
- Cup of broth or soup that has been strained
- Cup of fruit juice
- Yogurt
- Glass of water
Evening Snack
- Ice cream or frozen yogurt
- Warm cocoa
- Glass of water
3 weeks to up to 6 weeks after surgery; A soft food diet
After the pain subsides, you will feel more capable of transitioning from a liquid diet to a soft food diet. During the weeks and months following surgery, it is vital to remember that your jaw is still mending and the implants are attempting to integrate.
The process by which the jaw creates a biological bond with the implant screws is known as osseointegration. To ensure that this occurs correctly, you must continue to monitor your diet.
During the inital three months, you MUST avoid consuming meals that are - heard, chewy or crunchy and that require less chewing.
What foods may I consume during this time?
After three weeks, the following are examples of things you can add to your diet;
- Anything that is mashed or puréed, such as - mash potato, fruits, vegetables
- Everything soft, such as - bananas and melons
- Everything in a can and lacking skin and seeds
- Anything baked or cooked to a tender texture
- Soft breads, cakes
- Cooked pasta (soft)
- Noodles
- Quinoa, cous cous
- Eggs - poached, scrambled
- Pureed sauces
Example Menus for three weeks to six weeks:
This is a sample menu for a one-day soft food diet after surgery. It is vital to note that you should have snacks to ensure that you receive the necessary nutrients and calories for recuperation.
Breakfast
- Scrambled eggs on soft bread
- Fruit juice or smoothie
- Cup of tea or coffee
- Yogurt
- Glass of water
Breakfast Snack
- Bowl of soft fruit
- Glass of fruit juice
- Glass of water
Lunch
- Soup
- Stir fry with soft vegetables and noodles
- Jelly
- Soft fruits
- Glass of water
Dinner
- Meat cooked to a tender texture with mashed potato
- Cup of fruit juice
- Soft cake wirh custard or cream
- Glass of water
Several Important Suggestions for the Recuperation Period
Utilize a food blender or processor. If you can combine some of your favourite foods, you can better appreciate the fluid/soft food diet restrictions during the first several weeks of recuperation.
If you enjoy your food, you are more likely to consume sufficient calories and nutrients to help the healing process. Take initiative. When you decide to undergo this procedure, begin investigating what foods you can and cannot consume. This can include recipes for various shake and smoothie varieties. This can also help you stock up on food before surgery so that you are prepared to eat after you get home to recover.
Observe your body. Adjust your intake if you ever feel like you are not getting enough or are perhaps getting too much. Ask relatives for support. And get ~plenty of rest.
How about...
What about unmentioned details? You have learnt primarily what meals you can eat and a small amount about those you should avoid. But there are certain foods and beverages that we are commonly questioned about;
- Do not consume nuts or similar items - these will be far too hard and crunchy for your jaw
- Avoid hot and spicy liquids 24 to 48 hours after the surgery
- During the recovery phase, excessive alcohol consumption should be avoided, as alcohol consumption can impair the dental implants.
You can always consult the dental surgeon should you have any enquiries.
A budget alternative to fixed full jaw implant prosthesis is a snap on denture (over-denture) starting from £3000. By Dr Amir Mostofi DDS, Dip. , MSc.
Overdentures, also referred to as snap-on dentures, are a type of denture that attaches to a few dental implants placed in the jaw bone. Compared to conventional dentures, they have a number of advantages, such as better stability, retention, and a more realistic bite. Additionally, they offer increased durability, do not need adhesives, and aid in maintaining the jaw bone. The price range begins at £2500.
**A budget alternative to fixed full jaw implant prosthesis is a Snap-on denture (overdenture) starting from £3000.By Dr Amir Mostofi DDS, Dip. ,MSc. **
Snap-on dentures (also called implant-retained or implant overdentures) are removable dentures that “click” onto implants. They’re often chosen as a more affordable option compared with fully fixed full-arch implant bridges, while still giving far better stability than conventional dentures.
Typical UK price ranges ( 2026 guide at the time of writting)
Costs vary depending on the number of implants and whether a bar is used:
2 implants: £3,000 – £4,000
4 implants: £4,000 – £7,000
Optional metal bar: add around £1,000
These fees typically include consultation, X-rays/planning, implants, and the denture. For an up to date price see our fee page.
Ongoing maintenance costs
Implants need long-term maintenance, and the denture attachments will wear over time. Plan for:
Annual review and hygiene/cleaning around implants (recommended at least once per year)
Replacing the plastic retention inserts inside the denture: typically £60 – £200 (depending on type/how many)
Repairs/adjustments if needed (we always discuss costs before proceeding)
Alternatives to snap-on dentures
Depending on your goals and budget, alternatives include:
Conventional dentures (lower cost, but typically less stable)
All-on-4 type fixed teeth (fixed bridge supported by implants)
Fixed implant bridge (non-removable option in suitable cases)
Some patients would like to have a full jaw implant restored fixed prosthetics. However, the cost of such treatment is beyond their reach. The cost of fixed dental implants for a full jaw restoration can vary depending on several factors, such as the number of implants needed and the experience level of the surgeon. However, on average, a fixed full jaw restoration with fixed dental implants can cost between £10000 to £25000 (at the time of writting) in UK. A practical alternative is option of overdenture (snap on denture). The cost of Snap-on dentures for a full jaw restoration is typically less expensive. The cost can vary depending on the number of dental implants needed and the materials used for the denture. However, on average, the cost for a full jaw restoration with a Snap-On denture can range from £3000 to £8000 in United Kingdom. This cost is more affordable for many patients.
Snap-on dentures, also known as overdentures, are a type of denture that snaps onto a small number of dental implants in the jaw bone. This type of denture offers a number of benefits over traditional dentures, which rest on the gums and are held in place by suction or adhesives.
One of the main benefits of snap-on dentures is improved stability and retention. Traditional dentures can slip and move around in the mouth, causing discomfort and making it difficult to speak and eat. Snap-on dentures, on the other hand, are securely attached to the dental implants, which anchor them firmly in place. This means that snap-on dentures do not slip or move around in the mouth, which greatly improves the ability to speak and eat.
Another benefit of snap-on dentures is that they provide a more natural-feeling bite. Traditional dentures can change the way the jaw and teeth align, which can cause discomfort and even jaw pain. Snap-on dentures, however, are anchored to the jaw bone, which helps to maintain the natural alignment of the jaw and teeth. This can help to reduce discomfort and jaw pain.
Another benefits of snap-on dentures is that they do not require adhesives to hold them in place. Traditional dentures rely on adhesives to keep them in place, which can be messy and unpleasant to use. Snap-on dentures, on the other hand, are anchored to the jaw bone and do not require adhesives to stay in place. This makes them more convenient and comfortable to wear.
In addition, snap-on dentures can help to preserve the jaw bone. Traditional dentures rest on the gums and rely on suction to stay in place. Over time, this can lead to bone loss in the jaw, which can cause the dentures to fit poorly and make the face appear sunken. Snap-on dentures, however, are anchored to the jaw bone and help to preserve bone and maintain a more youthful appearance. Snap-on dentures, also known as overdentures, are a more cost-effective option for full jaw restoration compared to fixed dental implants. While both options can provide a secure and stable solution for missing teeth, the cost of fixed dental implants can be significantly higher.
Another factor to consider is the maintenance costs. Fixed dental implants require regular check-ups and cleaning like natural teeth, but snap-on dentures are easy to clean and maintain, which can save patients on additional costs in the long run.
It's worth noting that the final cost of the treatment will depend on the individual case, and it's important to consult with a dental professional to get an accurate estimate of the cost. In conclusion, Snap-On dentures offer a number of benefits over traditional dentures, including improved stability and retention, a more natural-feeling bite, greater durability, no need for adhesives, preservation of jaw bone, more budget friendly and easy to clean. While they may require more upfront costs, snap-on dentures are a more secure, durable, and comfortable option for those in need of dentures.
Book an assessment in Worthing
If you’d like to know which option suits you best, we can assess you and provide a clear plan and estimate.
Call: 01903 821822
Address: 7 Chapel Road, Worthing, West Sussex BN11 1EG
Or use the website contact/booking page.
What are differences between fully acrylic and Cobalt- Chrome dentures? - By Dr Amir Mostofi DDS, Dip. MSc.
The goal of dentures is to give patients a set of teeth that both look and function naturally. In terms of the components they are made of, their degrees of strength, and their prices, they vary significantly. Cobalt-chrome dentures are made from a combination of cobalt and chromium, while fully acrylic dentures are made entirely of acrylic resin. Dentures made of cobalt-chrome are more resistant to temperature changes than those made entirely of acrylic, which can break if exposed to extremely cold or hot temperatures. Dentures made of cobalt- chrome are more robust and long-lasting, but they are also more expensive and can sometimes induce allergic reactions in some people.
What are differences betwen fully acrylic and Cobalt- Chrome dentures?
Choosing between an acrylic denture and a cobalt chrome denture can make a big difference to comfort, stability, and how long your denture lasts. In this guide we compare acrylic vs cobalt chrome in plain English, including pros/cons, typical use-cases, and how to choose the right option for your mouth.
If you’d like a personalised recommendation, you can book a denture assessment at our Worthing clinic: Call 01903 821822 or use our contact page.
Two types of dentures are utilised to replace missing teeth: fully acrylic and cobalt-chrome dentures. Although they are both intended to provide patients a set of teeth that looks and functions naturally, they differ significantly in terms of the materials they are made of, their levels of strength, and their costs.
The material used to produce entirely acrylic and cobalt-chrome dentures is one of their primary distinctions. Fully acrylic dentures are built entirely of acrylic resin, a lightweight, user-friendly synthetic polymer. Conversely, cobalt-chrome dentures are constructed from a mix of cobalt and chromium, both of which are robust and long-lasting metals.
The strength and endurance of the two varieties of dentures is another difference. Since the metal used in their manufacture is more harder and more resistant to wear and tear, cobalt-chrome dentures are often stronger and more long-lasting than completely acrylic dentures. On the other hand, completely acrylic dentures are vulnerable to fracturing or cracking if not treated correctly.
The price of completely acrylic dentures is one of their benefits. They are a more cost-effective solution for patients on a tight budget because they are often less expensive than cobalt-chrome dentures. Since the acrylic material can be easily moulded and moulded, they are also simpler to repair and modify.
Cobalt-chrome dentures, on the other hand, have some definite advantages of their own. Since they are lighter and thinner than totally acrylic dentures, they are more comfortable to wear. Furthermore, they offer a more natural feeling in the mouth due to their snugger and more secure fit. Cobalt-chrome dentures are moreover less prone to yellowing and staining, making them simpler to maintain and retain appearing clean and new.
Cobalt-chrome dentures also have the benefit of withstanding drastic temperature changes. Cobalt-chrome dentures are more resistant to these temperature variations than fully acrylic dentures, which can become brittle and break if exposed to extremely cold or hot temperatures. They are therefore a better option for those who reside in regions with large temperature swings.
Fully acrylic dentures' propensity to break or crack is one of its main drawbacks. They are also prone to yellowing and staining, which can be challenging to remove. Additionally, they could deteriorate more quickly than cobalt-chrome dentures and need to be replaced more frequently.
Dentures made of cobalt-chrome also have significant drawbacks. The fact that they are typically more expensive than totally acrylic dentures is one of their key disadvantages. Due to the tougher and less flexible nature of the metal used in their production, they are also more challenging to repair or change. Additionally, certain persons who are allergic to cobalt or chromium may experience allergic reactions when wearing cobalt-chrome dentures.
Acrylic vs Cobalt Chrome Dentures: Quick Comparison
Acrylic dentures (plastic):
- Usually lower cost
- Quicker to adjust/repair
- Often used for temporary or simpler partial dentures
- Can be bulkier and may feel less stable in some cases
- May be more prone to fracture over time (depending on design)
Cobalt chrome dentures (metal framework):
- Typically thinner and more rigid
- Often feel more secure with better support
- Can be more comfortable due to reduced bulk
- Common choice for partial dentures where teeth remain
- Usually higher cost and more technical to manufacture/alter
In conclusion, cobalt-chrome and completely acrylic dentures each have specific benefits and drawbacks. Fully acrylic dentures are typically less expensive and simpler to fix, but they are less sturdy and more likely to shatter or crack. Dentures made of cobalt-chrome are more robust and long-lasting, but they are also more expensive and can sometimes induce allergic reactions in some people. The greatest option for a patient will ultimately rely on their specific requirements and financial situation.
Which one is best for me?
You may be better suited to acrylic if:
you need a lower-cost option
it’s a temporary denture (e.g., after extractions)
you expect changes and want something easier to adjust
You may be better suited to cobalt chrome if:
you want a slimmer, stronger partial denture
you have enough healthy teeth for a stable design
you want better longevity and stability for chewing
A clinical assessment is important because gum support, bite forces, and remaining teeth all affect the best design.
Book a denture assessment in Worthing
If you’re unsure whether acrylic or cobalt chrome is right for you, we can assess your mouth, discuss options, and provide a clear plan.
Call: 01903 821822
Address: 7 Chapel Road, Worthing, West Sussex BN11 1EG
You can also contact us online via the website contact page.
"Dental Bite Splints: A Comprehensive Guide to Relief, Protection, and Improved Oral Health" - By Dr Amir Mostofi DDS, Dip. MSc
A dental bite splint is a small, detachable device worn over the teeth to assist reduce pain and suffering brought on by bruxism, TMJ disorders, and other abnormalities with the bite. These splints can be tailored to fit a person's mouth and are often constructed of acrylic or other hard plastic materials.
Bruxism is a condition in which a person unintentionally clenches or grinds their teeth, frequently when they are asleep. Numerous issues, such as tooth deterioration, jaw pain, migraines, and facial muscle pain, may result from this. In order to reduce pressure and strain on the jaw muscles and joints, which can cause pain and discomfort, bite splints work by giving the teeth a smooth, even surface to rest on.
What are dental bite splint?
A dental bite splint is a small, detachable device worn over the teeth to assist reduce pain and suffering brought on by bruxism, TMJ disorders, and other abnormalities with the bite. These splints can be tailored to fit a person's mouth and are often constructed of acrylic or other hard plastic materials.
Bruxism is a condition in which a person unintentionally clenches or grinds their teeth, frequently when they are asleep. Numerous issues, such as tooth deterioration, jaw pain, migraines, and facial muscle pain, may result from this. In order to reduce pressure and strain on the jaw muscles and joints, which can cause pain and discomfort, bite splints work by giving the teeth a smooth, even surface to rest on.
The jaw joint and the muscles that govern the jaw are both impacted by TMJ disorders. These conditions can make it difficult to bite and chew, as well as create pain and discomfort in the jaw, cheeks, neck, and shoulders. By helping to stabilise the jaw and redistribute the power of biting and chewing, bite splints can assist to reduce these symptoms.
Bite splints come in a variety of designs and forms, each with a distinct function. Hard splints, soft splints, occlusal guards, and orthopaedic splints are the most popular varieties. Hard splints are designed to offer a sturdy surface for the teeth to rest on and are composed of acrylic or other hard plastic materials. They are typically worn at night and can aid in reducing bruxism and TMJ disease symptoms. On the other side, soft splints are created to be more comfortable to wear and are constructed of softer materials like silicone or rubber. They are typically worn during the day and offer a temporary fix for people who have dental work or missing teeth, as well as relief from the signs and symptoms of bruxism and TMJ disorders. In order to protect the teeth from harm when participating in sports or other physical activities, occlusal guards are similar to hard splints. Orthopedic splints, on the other hand, can be worn for a longer amount of time and are intended to assist address misaligned bites or other abnormalities with the bite.
Each patient's bite splint is normally constructed specifically for them by a dental practitioner. To identify the root of the patient's bite issues, the procedure starts with a dental examination and bite analysis. The dentist will then make a model of the patient's mouth using impressions of the patient's teeth. The bite splint is then created using the model as a guide and materials and methods tailored to the patient's requirements.
The usage of a bite splint has several advantages, including the reduction of pain and suffering brought on by bruxism and TMJ conditions, defence against teeth grinding and clenching, stabilisation of the jaw and correction of misaligned bites, and enhancement of sleep. However, using a bite splint has some potential drawbacks as well, such as initial discomfort while getting used to wearing the splint, difficulty speaking or eating while wearing the splint, the need for routine cleaning and maintenance of the splint, and the potential for tooth movement or changes in the bite if the splint is not properly fitted or maintained.
A dental bite splint is an effective tool for people who suffer from pain and discomfort brought on by teeth grinding, TMJ disorders, and other bite-related problems. These splints can offer comfort, safeguard teeth, and enhance general dental health. If a biting splint is the best course of therapy for you, it's crucial to speak with a dentist who can also correctly fit and maintain the splint to maximise its effectiveness.
While bite splints can frequently help with the pain and discomfort brought on by bruxism and TMJ issues, it's crucial to treat the underlying issue if you want to experience long-lasting relief. This may entail dietary adjustments, stress reduction measures, or the application of additional therapies like mouthguards or dental appliances.
It's critical to maintain appropriate dental hygiene while wearing a biting splint in addition to treating the underlying causes of bite issues. To do this, you should frequently brush your teeth, floss them, and visit a dentist for cleanings and checkups. To ensure their efficiency and durability, bite splints should also be frequently cleaned and stored in a safe place when not in use.
If any discomfort or problems develop while using a bite splint, it is extremely crucial to speak with a dental expert. If the splint is not offering the required relief or if it is causing any discomfort or problems, it may need to be changed or replaced.
Although bite splints can be a beneficial therapy choice for many patients, they might not be appropriate for all patients. Before beginning use of a bite splint for treatment, it is crucial to discuss any worries or queries with a dental practitioner.
Bite splints can improve general oral health in addition to reducing pain and discomfort. Bite splints can assist to prevent tooth damage and maintain the health of the teeth and gums by shielding the teeth from clenching and grinding. Additionally, they can aid in jaw stabilisation and bite alignment correction, enhancing the mouth's overall functionality and attractiveness.
In general, bite splints can be a helpful therapy choice for those who are in pain or uncomfortable due to teeth grinding, TMJ disorders, or other bite-related problems. Although utilising a biting splint may have some downsides, for many people, the advantages of comfort and better oral health may outweigh these concerns. To ensure the success of the bite splint, it is crucial to work closely with a dental professional to choose the best course of treatment and to properly fit and maintain the appliance.
Conscious Sedation in Dentistry. By Dr Amir Mostofi DDS, Dip. MSc
Conscious sedation is a type of dental treatment that involves the use of medication to help patients relax during procedures. This type of sedation allows patients to remain awake and able to respond to instructions from the dentist, but they may feel drowsy and relaxed. The use of conscious sedation in dentistry has several benefits, including helping patients who experience anxiety or fear during dental procedures feel more relaxed and comfortable. There are several different types of medications that can be used for conscious sedation, including oral, inhaled, and intravenous (IV) options. Conscious sedation is typically administered and monitored by a trained professional to ensure the patient's safety and comfort.
Conscious Sedation In Dentistry.
Conscious sedation is a type of dental treatment that involves the use of medication to help patients relax during procedures. This type of sedation allows patients to remain awake and able to respond to instructions from the dentist, but they may feel drowsy and relaxed.
The use of conscious sedation in dentistry has several benefits. For patients who experience anxiety or fear during dental procedures, conscious sedation can help them feel more relaxed and comfortable. This can make it easier for the dentist to perform the procedure, and can also help the patient avoid feelings of distress or discomfort.
There are several different types of medications that can be used for conscious sedation in dentistry. The most common type is oral sedation, which involves taking a pill before the procedure. This type of sedation can provide a moderate level of relaxation, and can be adjusted to meet the individual needs of the patient.
Another type of conscious sedation is inhaled sedation, also known as laughing gas. This involves inhaling a mixture of nitrous oxide and oxygen through a mask placed over the nose. Inhaled sedation provides a mild to moderate level of relaxation, and the effects can be quickly reversed by breathing pure oxygen.
Intravenous (IV) sedation is another option for conscious sedation in dentistry. This involves administering the medication directly into the bloodstream through a vein, allowing the dentist to carefully control the level of sedation. IV sedation can provide a deeper level of relaxation than oral or inhaled sedation, but it also carries a higher risk of complications.
Regardless of the type of medication used, conscious sedation in dentistry is typically administered and monitored by a trained professional. The dentist or sedation provider will carefully assess the patient's medical history and condition to determine the appropriate dosage and type of medication. They will also monitor the patient's vital signs throughout the procedure to ensure their safety and comfort.
Overall, conscious sedation is a safe and effective way to help patients relax during dental procedures. It can make the experience more comfortable for patients who experience anxiety or fear, and can also make it easier for the dentist to perform the procedure. Patients who are interested in conscious sedation should talk to their dentist to learn more and determine if it is right for them.
Clinic for Implant & Orthodontic Dentistry is located in the heart of Worthing and offers all forms of dental treatments under sedation to anxious patients older than 12 years. Patients under the age of 12 must be referred to the country's specialised sedation centres.
Is there a relationship between root canal and cancer? - By Dr Amir Mostofi DDS, Dip. MSc
There is no direct relationship between cancer and root canal treatment. Root canal treatment is a common dental procedure performed to save a tooth that has been damaged or infected, while cancer is a disease caused by the uncontrolled growth of abnormal cells in the body. Good oral hygiene and overall health habits can help to prevent the need for root canal treatment and reduce the risk of cancer.
There is no direct relationship between root canal treatment and cancer. However, it is important to understand the role of root canal treatment in maintaining oral health and how this can affect overall health, as well as the potential risks and complications associated with the procedure.
Root canal treatment is a common dental procedure that is performed to save a tooth that has been damaged or infected. The goal of the treatment is to remove the infected or damaged tissue from inside the tooth, called the pulp, and to clean and seal the inside of the tooth to prevent further infection. The pulp of the tooth contains nerves, blood vessels, and other tissues that help the tooth to grow and develop. When the pulp becomes infected or damaged, it can cause pain, swelling, and other symptoms that can affect the health of the tooth and the surrounding tissues.
Root canal treatment is typically recommended when the pulp of a tooth becomes infected or damaged. This can happen for a variety of reasons, including tooth decay, trauma to the tooth, or a crack or chip in the tooth. In some cases, the infection or damage to the pulp may be severe enough to cause an abscess, which is a pocket of pus that forms at the end of the root of the tooth. If left untreated, an abscess can spread the infection to other parts of the mouth and body, and can cause serious health complications.
The procedure for root canal treatment involves removing the infected or damaged pulp from the inside of the tooth, cleaning the inside of the tooth, and filling and sealing the empty space. This is typically done under local anesthesia to numb the area and prevent pain. The tooth may also be fitted with a crown or other type of restoration to protect it and restore its function.
While there is no direct relationship between root canal treatment and cancer, there are some potential risks and complications associated with the procedure. For example, the procedure can sometimes be painful, and there is a small risk of infection or damage to the surrounding tissues. In rare cases, the tooth may not heal properly or may become re-infected, requiring additional treatment.
It is important to maintain good oral hygiene and to visit the dentist regularly for checkups and cleanings in order to prevent the need for root canal treatment and to reduce the risk of complications. This includes brushing and flossing daily, avoiding sugary and acidic foods and drinks, and avoiding tobacco and excessive alcohol consumption.
In conclusion, while there is no direct relationship between root canal treatment and cancer, the procedure is an important part of maintaining oral health and can prevent the spread of infection and other health complications. It is important to practice good oral hygiene and to visit the dentist regularly in order to prevent the need for root canal treatment and to reduce the risk of complications. Overall, taking care of your oral health is an important part of maintaining overall health and well-being.